The Ever-Present and Ever-Important Intersection of Public Health and Medicine
Written by: Gautam Naik | Edited by: Ben Segev
“Medicine”. “Health”. “Safety”. All of these words are synonymous with people’s perception of the medical field and the work of clinicians. When people hear the word “treatment”, they think of someone with an MD or in scrubs. However, an equally important field that mirrors the goals of traditional medicine is public health, an area of medicine I was first introduced to with PBHLTH 116 during my second semester at Berkeley. Public health takes such a varied approach to solve prevalent health issues in the community; yet, it is so relevant to medicine that neither can be discussed independently of each other. If this didn’t really make sense, let me explain with an analogy: imagine a scenario where the issue in society is that the babies are constantly put into the river. With the “medical approach,” you would focus on saving the babies from the river. In essence, you are reacting to the problem after it has happened. With the “public health approach,” you would focus on preventing the babies from being put in the river in the first place. In essence, you are dealing with the problem before it even occurs. Both approaches answer the same question, but do so through different lenses. Originally, I focused on attending med school, earning my MD, and contributing to my community through the traditional medical approach. However, getting exposed to the public health side of medicine really opened my eyes to the vast possibilities in the medical field—beyond those presented by the traditional approach alone. Additionally, I learned the importance of combining every aspect of healthcare in order to create a balanced approach to tackle health issues.
The academic career path we follow is always centered around the kinds of questions we ask and the answers we find. Before being introduced to public health, the questions that I asked were synonymous to those commonly found in the traditional medical field. What can be done to mitigate negative outcomes? What treatments can help cure people or manage symptoms of different illnesses? However, after taking PBHLTH 116 and hearing experts discuss their work in fields ranging from violence to reproductive justice to bioethics, the questions I began to ask deepened. It no longer just became about what can be done to treat symptoms and illnesses. It became about “why diseases are more prominent in certain communities?” and “how can people be kept safe in the first place?” Disease prevention became just as important to me as disease intervention.
I chose to write this article because sometimes the field of public health can go unnoticed in comparison to the conventional medical field. Its importance and impact on medicine can often be neglected, even though it is ever present. Their intersection was most recently highlighted during the pandemic, when public health policies attempted to stem the spread of the virus while the traditional medical approach worked towards developing vaccines and a treatment plan for COVID-19. As we all work towards building our medical knowledge for our future in the field, it is important to be aware and knowledgeable of the public health side of things to be in a more able position to truly better the lives of those we serve. I had mentioned at the beginning of this article that neither public health nor the traditional view of medicine can be discussed independently of each other. To further elaborate, public health is like a lens over our medical perspective. It allows us to see a 2D scenario in 3D, being able to understand the circumstances from different perspectives. Ultimately, public health is worth investing your time in because it will help you be a more aware clinician. It will no longer just be about the disease or injury you are treating. It will also be about the patient behind the injury and the circumstances that led to their visit.
Additional Resources:
Introduction to Public Health|Public Health 101 Series|CDC
What the Experts Want Us to Know About Public Health
2024 Spring PBHLTH 116 001 LEC 001
2024 Spring PBHLTH 24 001 SEM 001
Unlocking Hope: Advancements in Alzheimer’s Research
Written by: Allen Justin | Edited by: Ben Segev
Alzheimer’s disease (AD) remains one of the most challenging frontiers in medical research, affecting millions worldwide. In recent years, the pursuit of effective treatments and potential cures has intensified, leading to promising breakthroughs and innovative approaches that provide a glimmer of hope for those impacted by this devastating condition. Let’s delve into the latest advancements in Alzheimer’s research and the potential they hold for transforming the landscape of AD treatment.
1. Reassessing the Amyloid Hypothesis:
The traditional amyloid hypothesis, which posits that the accumulation of beta-amyloid plaques is the primary driver of AD, has faced scrutiny. Recent research suggests that solely targeting amyloid may not be sufficient for meaningful clinical improvement. The emphasis has shifted to exploring alternative pathways, with a particular focus on the role of tau protein.
2. Tau-Targeted Therapies:
Unlike the disappointment seen with anti-amyloid treatments, therapies targeting tau pathology have gained momentum. Tau, a microtubule-associated protein, forms twisted tangles within nerve cells in the brains of individuals with AD. Emerging preclinical and animal studies indicate that reducing tau levels may be associated with improved cognitive performance, fostering optimism for the development of tau-targeted therapies.
3. Immunotherapy Innovations:
Immunization studies, both against amyloid and tau, are at the forefront of AD research. Early clinical trials have explored vaccines aimed at reducing intracellular levels of tau, offering a glimpse of potential cognitive benefits. As these studies progress, the prospect of harnessing the immune system to combat AD is becoming increasingly tangible.
4. Precision Medicine Approaches:
The diversity in how Alzheimer’s manifests in individuals underscores the importance of personalized approaches. Precision medicine, tailoring treatments based on an individual’s
genetic makeup, lifestyle, and unique characteristics, is gaining traction. This individualized strategy holds the potential to maximize therapeutic efficacy while minimizing side effects.
5. Early Detection and Biomarkers:
Timely detection remains a critical factor in managing Alzheimer’s disease. Advances in neuroimaging and biomarker research are paving the way for identifying early signs of AD, even before noticeable symptoms appear. This early diagnosis facilitates the implementation of interventions when they are likely to be most effective.
6. Leveraging Technology for Cognitive Health:
Digital therapeutics and cognitive training programs are leveraging technology to support cognitive health in individuals at risk of or diagnosed with AD. Apps and platforms designed to enhance memory, attention, and problem-solving skills are being explored as complementary tools in the management of Alzheimer’s.
7. Drug Repurposing and Combination Therapies:
Researchers are investigating existing drugs approved for other conditions to identify potential candidates for repurposing in Alzheimer’s treatment. Additionally, combination therapies that target multiple aspects of the disease simultaneously are being explored for enhanced efficacy. One example of drug repurposing for Alzheimer’s disease is the investigation of the anti-diabetic drug, pioglitazone. Pioglitazone is an FDA-approved medication used to treat type 2 diabetes. It belongs to the class of drugs known as thiazolidinediones and works by improving insulin sensitivity in the body. Researchers however have been exploring the potential neuroprotective effects of pioglitazone in Alzheimer’s disease. Some studies suggest that pioglitazone may have anti-inflammatory and anti-oxidative properties, which could be beneficial in reducing neuroinflammation and oxidative stress—both of which are implicated in Alzheimer’s pathology.
8. Gene Editing Breakthroughs:
Advances in gene-editing technologies, such as CRISPR-Cas9, offer unprecedented opportunities to address the genetic components of Alzheimer’s disease. While still in early
stages, gene-editing research holds promise for modifying or eliminating genetic factors associated with increased risk.
9. Conclusion:
The landscape of Alzheimer’s research is undergoing a shift, fueled by innovative approaches and a deeper understanding of the disease’s complexities. While a definitive cure remains elusive, the progress in tau-targeted therapies, immunotherapy, precision medicine, and technological interventions brings forth a new era of hope for individuals and families affected by Alzheimer’s disease. As research continues to unravel the intricacies of AD, the collaborative efforts of scientists, clinicians, and the global community hold the key to unlocking breakthroughs that may change the trajectory of this devastating condition. As we navigate the promising advancements in Alzheimer’s research, the prospect of a brighter future for those affected becomes increasingly tangible
Sources:
Giacobini, E., Gold, G. Alzheimer disease therapy—moving from amyloid-β to tau. Nat Rev Neurol 9, 677–686 (2013).
https://doi.org/10.1038/nrneurol.2013.223 Wendy Noble, Maria Jimenez-Sanchez, Beatriz G. Perez-Nievas & Diane P. Hanger (2020) Considerations for future tau-targeted therapeutics: can they deliver?, Expert Opinion on Drug Discovery, 15:3, 265-267, DOI: 10.1080/17460441.2020.1685977
A Sample of Medical Scribing
Written by: Yichen Zeng | Edited by: Ben Segev
Whether it be clinical volunteering, shadowing, or hospital internships — with so many options at our disposal these days for glimpsing into the day-to-day lives of physicians, it’s quite difficult for pre-med students to determine for themselves which of these opportunities suits their interests and career goals the most.
One particular opportunity that many pre-meds may be aware of but not as many genuinely consider is the role of a medical scribe. Medical scribing is the documentation of patient encounters on behalf of some clinician; in other words, as a scribe, you would follow a doctor around as they treat their patients and update patients’ electronic health records with the patients’ subjective histories, the doctor’s physical exam results, and the doctor’s proposed treatment plans for their patients. As medical records become increasingly complex and tricky to navigate, medical scribes are becoming in higher and higher demand; with scribes, doctors are able to concentrate more on interacting with their patients instead of wasting their and their patients’ time on trudging through clerical duties.
At a glance, medical scribing appears to be the perfect opportunity for pre-meds to gain clinical experience! Not only does medical scribing enable students to step into the shoes of a physician and immerse themselves in the workplace dynamics of a clinic, but also it requires students to take on one of the primary responsibilities of a doctor — which will eventually become one of their primary responsibilities once they begin practicing.
Yet, in select circles of pre-med students and advisors, medical scribing is viewed rather negatively. Why is this the case? Well, those who view medical scribing as less beneficial for pre-meds than other clinical opportunities often argue that medical scribing doesn’t provide students with the invaluable experiences from interacting directly with patients. However, this argument is rather misleading: while it is true that scribes are, at most hospitals and clinics, prohibited from performing medical services or offering medical advice to the patients they meet, they are absolutely permitted (and even encouraged) to socialize with their patients casually. This can range from exchanging pleasantries to inquiring into the patients’ lives if the patients are eager to disclose some recent exciting developments in their lives. Both of these activities hone skills that doctors must acquire and perfect in order to be successful at forging lasting interpersonal relationships with their patients.
For prospective medical scribes or pre-meds who are interested in this route of acquiring clinical experience, the onboarding process — which is that of a formal employment — may seem daunting and perplexing at first. Fortunately though, past the mountains of paperwork, the process is quite straightforward: both classroom training and floor training (that is, training outside of the classroom and in the medical offices at which scribes-in-training intend to work), while intensive, are rather short in duration. In fact, often only a month or two elapse between the submission of the job application and the first day of work.
One popular employer of medical scribes is ScribeAmerica, a provider of medical scribes to various medical practices around the country. Under ScribeAmerica, classroom training usually lasts several weeks and involves the memorization and comprehension of basic anatomy and physiology while floor training lasts for around a month or so. ScribeAmerica’s popularity can largely be attributed to the convenience of onboarding and the company’s expansive nationwide footprint.
For most students like me who are still in school, we elect to accept a part-time position: with ScribeAmerica, that entails a minimum of twenty hours per week which, while certainly gruesome at times, will provide clinical exposure and experiences that are extremely pertinent to the career of a clinician and unique to the work of medical scribing. Moreover, ScribeAmerica is decently accommodating with their student employees; students can take time off for exams and emergencies without any repercussions. Though, like all employment, working as a medical scribe is a commitment that demands a consistent and dedicated approach.
Some medical scribes also work for hospitals directly or under other organizations and companies that provide similar services. Many students prefer those to ScribeAmerica due to higher pay or easier hours, though it is relatively more tedious to search for these opportunities simply because they are smaller in scale and coverage than ScribeAmerica.
For those of us who have yet to decide which option of gaining clinical experience is right for us, medical scribing is one that I would definitely recommend to consider. While the hours are long, they prepare us for the demanding hours that we may eventually work once we become doctors (and will work when we’re in residency). While the pay isn’t outstanding, it is at least an improvement from most other clinical opportunities that are purely volunteering in nature. And, of course, as a medical scribe, you’ll already have a foot in the door by the time you leave employment — a head start that will carry you far in your professional aspirations.
Being in a COVID Vaccine Trial
Written by: Kearston Stepenosky | Edited by: Arshad Mohammed
The later months of 2020 are stained in history as a painful period for much of the world. As the Covid-19 pandemic evolved, hospitals across the US stretched their capacity, more than 700,00 businesses closed, and more than 20 million jobs were lost. A glimmer in this disheartening time, however, was the approval of a vaccine on the horizon. At sixteen years old, I joined the first group of minors to enter the Pfizer Covid-19 vaccine trial. At the time, public enthusiasm to join that lineup was limited as parental fears of the vaccine’s effects stunted participation. Social distancing also disqualified many potential participants, as plausible exposure is critical for testing the drug’s efficacy. Having witnessed my dad participate in the adult trial, I was eager to observe this moment in medical history from the front row. As avid believers in the importance of medical research, my family supported me in joining the trial and my basketball team’s continued practice schedule meant I was still exposed to some degree, making me qualified.
Beyond the clearance process, the 24-month-long double-blinded study involved two injections, weekly surveys, routine phone calls, Covid tests, and antibody blood tests. A bout of body aches and chills following the initial injection made me hopeful I had received the vaccine rather than the placebo, and I later learned I was correct. Week after week, my phone alerted me through the TrialMax app to complete my trial screening, a series of questions about how I felt and whether I was experiencing Covid-like symptoms. My data, combined with the 753 other 16-17-year-old participants in the trial, informed researchers about potential symptomatic responses to the vaccine between our more formal check-ups.
As one singular statistic in such a major study, I viewed my role in the trial as impersonal but quickly learned that was not entirely the case. People in my life responded to my decision with a mixture of support and judgment, and I was surprised to discover the vastness of medical distrust in my community, something I hoped to combat. The opportunity to do so came in the form of media requests. Local papers reached out for interviews regarding my experience, as well as my dad’s. Painfully aware of the degree of vaccine hesitancy emerging, I enthusiastically agreed with the hope that linking a real child with support for the vaccine would de-escalate tensions. These media requests scaled from local outlets to larger sources like the LA Times, Inside Edition, National Geographic, and more. Though I was initially intimidated, I knew resistance to vaccinating children existed far beyond my city, and I wanted to help. I was asked about what fueled my decision to join and the importance of minors involving themselves in trials. I happily discussed the vitality of reopening schools and taking the steps to recover as a community, a message I hoped would resonate with people when coming from a student.
The vaccine, in my eyes, was key to ending the pandemic and to distrust it was to needlessly extend lockdown, mask mandates, and other precarious we have now largely graduated from. The aftermath of being interviewed involved a sea of hopeful reactions littered with inevitable criticisms about government tracking, infertility, and mutations from the lovely people of the internet. Months later, a young girl in the virtual afterschool cooking class I taught showed me my decision was worthwhile. As we ended for the day, she raised her hand and announced that her mom let her receive the vaccine after seeing me on TV. My hope from the beginning was to spread confidence in the vaccine, and this indicated a step in the right direction.
Ultimately, one of the things made most apparent to me by the distribution of the Covid-19 vaccine was the persistence of medical skepticism in modern society, especially as it applies to parenting. While those who refuse to vaccinate their children are undeniably guided by the belief that they are doing what is best for their family, it is almost always in conflict with viable research and to the detriment of the public. Sending a child to school unvaccinated is seemingly the viral equivalent of sending them underdressed into a snowstorm. The tension surrounding this topic makes it challenging to approach, but I see hope in how much of that tension stems from older generations. As people who grew up witnessing the ramifications of vaccine resistance and misinformation, it is my belief that we emerge as a motivated generation with high media literacy and faith in science.
By the time the pandemic declined, $814 billion in financial relief had been distributed and much of the population returned to school and work. The effects of this period, however, persist as flaws in healthcare, technology, resource distribution, and cleanliness have been illuminated. In the aftermath of this event, we as a society are left with a long list of what we may improve, and it is our participation in that growth, however small, that will make a difference.
Articles on my interviews!
- https://www.latimes.com/sports/highschool/story/2020-12-21/captain-calabasas-girls-basketball-team-pfizer-covid-19-vaccine-trial
- https://www.insideedition.com/meet-the-16-year-old-who-volunteered-with-dad-to-test-pfizers-covid-19-vaccine-63159
- https://spectrumnews1.com/ca/la-east/la-times-today/2020/12/02/cancer-survivor-and-his-daughter-join-coronavirus-vaccine-trial
- https://abc7.com/coronavirus-vaccine-clinical-trials-trial-volunteers-pfizer/8079563/
- https://scienceworld.scholastic.com/issues/2020-21/031521/testing-vaccines.html?language=english#1130L
- https://www.latimes.com/california/00000176-2563-d358-af7f-6d73d1be0000-123
- https://venturablvd.goldenstate.is/teen-vaccine-trial-volunteer-kearston-stepenosky/
Sources:
Art Therapy: A Brief History and its Effectiveness in Healing
Written by: Stephanie Kim | Edited by: Arshad Mohammed
As pre-med students, we are all too familiar with the importance of mental health and its impact on physical well-being. In recent years, there has been an increasing interest in alternative methods of therapy, such as art therapy, in treating mental health conditions. But what is art therapy, and how did it come to be? In this post, we will explore the history of art therapy and its effectiveness as a form of treatment.
Art therapy can be defined as a form of therapy that uses art as a means of expression and communication, in order to improve one’s mental health and emotional well-being. It is a type of therapy that combines psychotherapy and the creative process to explore thoughts, feelings, and emotions through the creation of art. For example, art therapy might involve a patient with anxiety being asked to create a piece of art that represents their anxiety. The therapist might then ask the patient to discuss their creation and the emotions it evokes, allowing the patient to explore their feelings and work through their anxiety. Art therapy might also involve a patient with PTSD being asked to create a series of drawings or paintings that represent their traumatic experiences. The therapist might then use these artworks to help the patient process their trauma and begin to heal. Furthermore, art therapy can be used in group settings, such as in schools or rehabilitation centers to allow patients to work on collaborative art projects, such as a mural or sculpture. Group art therapy can help build social connections and promote teamwork while also allowing participants to express themselves creatively.
The use of art as a means of healing dates back to ancient times, where it was used in various cultures as a form of expression and communication. In the 18th century, psychiatrists began to use art as a form of therapy to treat patients with mental illnesses. However, it wasn’t until the 1940s that art therapy was recognized as a legitimate form of treatment.
The pioneer of modern art therapy was Margaret Naumburg, a psychologist who introduced the concept of “art psychotherapy” in the early 20th century. She believed that art had the power to express unconscious thoughts and emotions, and that the process of creating art could help patients explore and understand their own feelings.
Since then, art therapy has evolved and is now used in a wide range of settings, including hospitals, schools, and rehabilitation centers. It is used to treat various mental health conditions, such as anxiety, depression, and PTSD, among others.
But what is the evidence behind the effectiveness of art therapy? Over the years, the effectiveness of art therapy in treating various mental health conditions has been supported by several studies. For instance, one study conducted by Pringle et al. (2011) found that art therapy was effective in reducing symptoms of anxiety and depression in adults with chronic illness. Participants in the study reported feeling less anxious and depressed after engaging in art therapy sessions, demonstrating the therapeutic benefits of this approach. Another study conducted by King et al. (2013) showed that art therapy was effective in reducing symptoms of PTSD in veterans. The study found that art therapy provided a safe and non-threatening space for veterans to express and process their trauma. Participants reported a reduction in the severity of their PTSD symptoms after engaging in art therapy sessions.
The benefits of art therapy go beyond just treating mental health conditions. It has also been shown to improve cognitive function, increase self-esteem, and promote self-awareness and self-expression. A review of the literature by Van Lith et al. (2015) found that art therapy had a positive impact on the cognitive function of adults with severe and enduring mental illness. Participants in the study reported improved cognitive skills, such as attention, memory, and problem-solving, after engaging in art therapy sessions. Additionally, the American Art Therapy Association (2020) notes that art therapy can increase self-esteem and self-awareness by providing patients with a creative outlet to explore and express their emotions.
Thus, art therapy is a powerful and effective form of treatment that has grown in recent years and is now recognized as a legitimate form of therapy. Art therapy provides patients with a creative outlet for their emotions and allows them to communicate in a nonverbal way, making it an effective form of treatment in improving cognitive function, increasing self-esteem, and promoting self-awareness and self-expression for those who may struggle with traditional talk therapy. By recognizing the importance of alternative forms of therapy, we can work towards a more holistic approach to healthcare that prioritizes the emotional and mental well-being of our patients. In the field of medicine, it is crucial to be open-minded and willing to explore new approaches to treatment, and art therapy is a prime example of the potential that alternative forms of therapy hold in improving the lives of patients.
Sources:
American Art Therapy Association. (2020). What is Art Therapy? Retrieved from https://arttherapy.org/what-is-art-therapy/
King, L. A., King, D. W., Fairbank, J. A., Keane, T. M., & Adams, G. A. (2013). Resilience-recovery factors in post-traumatic stress disorder among female and male Vietnam veterans: Hardiness, postwar social support, and additional stressful life events. Journal of Personality and Social Psychology, 104(5), 957–978. doi: 10.1037/a0031343
Malchiodi, C. A. (2012). Handbook of art therapy (2nd ed.). Guilford Press.
Pringle, B. A., Bunting, B. P., & Complementary Medicine Research Group. (2011). The effectiveness of art therapy interventions in reducing anxiety and depression in individuals with dementia: A systematic review and meta-analysis. The Journal of the American Medical Directors Association, 12(4), 306-310. doi: 10.1016/j.jamda.2010.08.002
Van Lith, T., Schofield, K., & Fenner, P. (2015). Art therapy for adults with severe and enduring mental illness: A review of the literature. The Arts in Psychotherapy, 42, 41-50. doi: 10.1016/j.aip.2014.12.004.
Debunking Premed Myths
Written by: Gautam Naik | Edited by: Arshad Mohammed
In order to debunk common pre med myths, I spoke with Mr. Hugo Mora-Torres, who is currently a pre med counselor at UC Berkeley. His knowledge regarding medical schools and their expectations comes from extensive training through the National Association of Advisors for Health Professionals (NAAHP), from weekly newsletters containing information from deans and admission committees of institutions, and from experience. Ultimately, the wealth of his knowledge is fact-based and not opinion-based.
- Being at a premier research institution, many premed students believe that they must be involved in research from their early years in order to be competitive during the medical school application process. What are your thoughts on this?
This is not true at all. While many students do pursue research while at Berkeley, it is in no way required as medical schools use a holistic review system during the application process. A model regarding the holistic review process can be found at the end of this Q&A along with a brief explanation of its different parts. Ultimately though, while research is in no capacity required to be competitive for medical school, it can serve as a great way to build various Attributes and Experiences. Through research, your critical thinking skills can grow and improve along with developing your quantitative reasoning, scientific inquiry, and written communication skills. Therefore, it does serve as a great way to grow as a student and to form relationships with professors and graduate students, which can be helpful for LORs during the application process.
- Often, premed students work hard to attain a flawless ‘A’ transcript, often sacrificing parts of their social life or mental health to do so, believing that all med students have such grades and that they are needed to be competitive. They believe that even one bad grade ruins your shot at medical school. Is this true?
Similar to my answer to #1, there is simply a baseline for GPAs and MCAT Scores. Once these thresholds are met, your Attributes and Experiences are considered. These aspects beyond grades help to determine if one has the capacity to be a good doctor. While grades show that one is intelligent, dedicated, and committed, it does not serve as an indicator or a guarantee that you will be a good doctor. As a result, your Attributes and Experiences are a big part of the process for admissions committees. While grades are not an end all be all, we should all have high academic standards in order to give us the best possible shot at medical school.
- In a bid to strengthen our resume and build medical experience, premed students can often sacrifice their other passions and hobbies, because they feel like it may not be valued by medical schools, like volunteering and clinical experience are the only things that matter. What is your opinion on this?
This is not the case at all. As long as your other hobbies and interests do not distract you from your medical ambitions, they are definitely important as an investment in activities shows commitment. This can help strengthen your attributes while simultaneously building great experiences that you can speak to during your application.
- Medical schools prefer premed applicants pursuing a science major (i.e. MCB, IB, MEB) over those pursuing a non-science major, because it shows they are more ‘committed’. Do med schools actually have a preference?
Medical schools do not have any preference whatsoever. Most premed students simply choose to pursue a science major like MCB or IB because many of their major requirements align with the prerequisites of medical schools.
- To be competitive for medical school, you have to spend your summers at a prestigious summer program or research institution. Simply volunteering or working at a clinic or other non profit organization is not enough. Is this the case?
Not necessarily. In your application, you must speak to the quality of the program and the impact it has had on you. Certain research programs do get funded by the NIH, so you might have richer experiences there. However, it must be a good fit. You can only have a quality experience that impacts you if you participate in a program or larger organization that aligns with your interests and provides great mentorship. More than worrying about how prestigious your summer program/activity may be, it is more important to first begin with a positive mindset geared towards learning and wanting to be challenged. This will allow you to utilize every opportunity given to you and build a rich summer experience. Finally, the richer the experience, the stronger an LOR your mentor will be able to write for you.
- For medical school, all you have to do is meet a certain level of participation in activities like volunteering or clinical experience. Once a certain amount of hours are performed, this will help your case for medical school, acting almost like a checklist.
Similar to #5, what matters is quality, not quantity. These activities aren’t just checkboxes on a form. They are experiences that help us grow into students and people that have the potential to be great doctors. During these experiences, a positive mindset, strong work-ethic, and extensive self-reflection is crucial to grow such that you become better prepared for medical school. Ultimately, more than just checkboxes, volunteering and clinical work are experiences geared towards helping us grow as students and as people to help us become more capable doctors.
- Medical schools view more ‘challenging’ majors as an advantage and will view poorer grades with more leniency. Is this true?
Not at all. Medical schools make no such differentiation. They view all grades the same despite your major, because the major you should be taking is the one that genuinely interests you. Therefore, medical schools show no sort of preference or increased leniency for ‘challenging’ majors, and, thus, challenging majors do not excuse poor grades.

The above model represents the holistic review process used by medical school admissions committees. In this model, there are three distinct parts: Metrics, Attributes, and Experiences
- Metrics→ These serve as a baseline. Once the minimum is met, the other two categories are considered.
- Attributes→ Primarily includes skills, personality, and traits. Considers how you have grown as a student and as a person throughout college and what you have gained.
- Experiences→ Considers general life experiences, including your time volunteering, doing clinical work, and conducting research (if applicable)
Importance of Fitness especially while being Pre-Med and increase efficiency, discipline, and improve mental health
Written by: Debora Ghosh | Edited by: Arshad Mohammed
You know when you sometimes have this sudden urge or inspiration that floods your mind? That’s what I had around the time of my birthday. I craved some consistency – a form of balance and structure. So, I decided to try going back to the gym. I used to go on and off before the pandemic but not consistently. Once I got to the gym, I was apprehensive and a little intimidated, confused as to what machines to use or not. Nonetheless, I tried out whichever machines were open for about an hour and returned home. That day, I decided that if I wanted to commit to his and pursue fitness, I was gonna go to the gym everyday for that week. I needed to create a habit, and eventually, I believed it would become a part of my routine. And that’s exactly what I did. It was pretty challenging, dragging myself to the gym after a long day of school and work, but I knew that my goals were not going to fulfil themselves. I wanted to get stronger, feel better,a nd develop this healthy habit. Eventually, I began to realize I needed to change up my eating habits and started making more high protein meals at home, or at least buying meals with more protein.
Before I knew it, I started feeling guilty if I did not go. How could I ever enjoy something that would leave me panting and huffing and puffing. Although at times, I went to the gym and was clueless as to what exercises to do and tried out random machines, at least I went. It was tough at times and often intimidating to go to the gym with people around me who seemed to know what they were doing. But, I learned to find comfort in the unknown. Beginning this journey elped me to step out of my comfort zone in an unprecedented way. Waves of thoughts such as “what if I am doing this exercise wrong” or “what if someone is judging me” flooded my brain. But, I tried to withstand these waves and realized that the gym was far from a judgemental place – everyone was simply working towards a better version of themselves. Not only did I feel like I had a newfound source of confidence, but I was able to get into the habit of going to the gym at a certain time of the day. This resulted in me having to block out chunks of my day and ensuring that I complete homework and other assignments to make time to go to the gym. Fitness had become an integral part of my life as it enabled me to become a more informed person about my physical and mental capabilities as well as limits. Pushing to failure on exercises such as hip thrusts or lat pulldowns encouraged me to strive towards greater goals in my academic life as well. This mindset of not giving up and persevering through struggles – whether it be an exercise or academic stress – had started to become a reality. From reducing my stress to staying more calm before midterms, coming to the gym felt like a sigh of relief, even through the 4 sets of 10 reps of sweat. Coming to the gym became an escape where I could focus on myself.
Seeing myself achieve personal records and fulfill goals helped me to feel more encouraged about my career goals as well. When I first attempted to do a pull-up, I was sure that I was never going to be able to get one. There was no way I could pull my body weight up – it seemed like an impossible feat. Gradually, however, I started with the assisted pull up machine, slowly making it harder and harder every week. Before I knew it, I was able to pull myself up, andI began to realize that my mind would often give up before my body could. The limits and apprehensions we create in our minds often restrict what we think our body can do.
Becoming a gym rat helped me to gain a newfound mindset that was fueled by discipline and consistency. Blocking out times to go to the gym helped me schedule studying and preparing for the MCAT too. I felt that prioritizing my own health and fitness goals strengthened my well-being and calmness. What I admired most about this journey is that progress is slow but once I started to see progress and achieve personal goals at the gym, this source of motivation translated into a greater sense of encouragement to achieving my career goals. This greater appreciation for the importance of lifestyle has informed me about what kind of physician I aspire to be in terms of being informed about patients’ lifestyles, cultures, and contexts.
What are Passion Projects?
Written by: Yichen Zeng | Edited by: Arshad Mohammed
Nothing quite encapsulates the spirit and drive of a physician more so than a Passion Project does! To be talented and skilled in that which we’re passionate about is wonderful in itself, but to use those passions and skills to uplift the community around us can often be far more fulfilling and meaningful. And, PMHS’s program for Passion Projects, which exactly utilize your unique set of values, talents, and goals to create a positive impact for the PMHS community and beyond, is perfect for aspiring physicians like us to begin our lifelong careers of altruism first at the local level!
While investigating how we could promote the awareness and encourage the undertaking of Passion Projects within the PMHS community, I interviewed Meeseo, the coordinator of and advisor for Passion Projects here at PMHS. Alongside her position as an officer of PMHS, Meeseo is currently participating in PMHS’s sole ongoing Passion Project: the Neurodiversity Awareness Project.
What constitutes a well-designed Passion Project? Well, Meeseo cites Down Syndrome Walk-a-thon, the volunteer campaign that was organized a few years ago to raise funds for Down Syndrome Connection of the Bay Area (a non-profit Down Syndrome organization), as the exemplary Berkeley-student-run philanthropic endeavor.
For one, Meeseo says, the project was highly accessible, both to the target community and those eager to become involved in operating and expanding this project; for one, the events were run asynchronously, i. e. participants were permitted to film and submit their participation whenever they had the time to. What’s more, while ordinary awareness projects tend to be more unidirectional in the sense that other projects really end at merely hollering into the vast abyss of social media and various political platforms without paying much attention to how the target communities are really benefiting from these projects, Down-to-Walk directly involved the communities it sought to uplift by enabling all participants – students, enthusiastic locals, and individuals with Down Syndrome – to come together for a cause that they cared about and witness the passion and contributions that others had towards their common cause on the project’s social media pages. Indeed, much of this project’s success should also be attributed to how well-advertised the project itself was on various social media platforms.
More general tips and advice for undertaking a Passion Project would include expecting a lot of logistical work. By “a lot,” Meeseo definitely means a lot: obviously, you have to contact lots of organizations regularly whether it’s to enlist their support or to request favors from them, but being able to connect well with people from all walks of life is no easy feat. Plus, rejections from those whom you contact for support will be common; “not being embarrassed” at rejections is a trait that teams behind any successful project must have, especially with how frequently you’ll be contacting third parties.
Finally, having a wealth of ideas for the directions in which your Passion Project can go would be extremely wise in order for your team to be flexible and accommodating with these third party organizations.
This transitions really well to tips and advice for those interested in launching their own Passion Projects but don’t quite know where to start. To be flexible and accommodating, you must first know your project – or at the very least what you hope to achieve with your project – inside out. Knowing whom you’d have to contact in order to expand and develop your project is also definitely crucial because they’ll, in the end, be as every part key to your project’s success as your team will be. Time management, as always, is an extremely necessary skill to have, but it’ll only become more necessary once you’re working with outside parties whose schedules won’t be as open to changes as a student’s might be.
But what if you don’t even know what exactly you hope to achieve with a Passion Project? Of course, that doesn’t mean that you can’t start brainstorming for ways to uplift your local community. As Meeseo advises, start by writing down ideas of what you’d like to accomplish – and you’re welcome to be as vague as you’d like! This is mainly so that you don’t forget about these ideas later, once you’ve compiled a list of decent size and begin deliberating over your next steps. Go through this list of ideas regularly to update them based on whatever new knowledge or insights you gain on their feasibility, necessity, or simply their appeal to you. Eventually, you’ll stumble across an idea that fits your interests and passions to a T, and from there, your Passion Project will germinate.
Is Neurosurgery as Amazing as I Imagined?
Written by: Yasmeen Medhat | Edited by: Arshad Mohammed
I was going into the hospital to shadow a neurosurgeon for the first time. I wasn’t sure what to expect–I had this idealized vision that neurosurgeons were these superheroes with steady hands and impeccable problem solving skills that fixed issues no other human on this planet could. I walked into the OR on my first day to find the attending I’m supposed to be shadowing sitting on her laptop in the corner of the room while two other individuals were performing the surgery; the surgery was a laminectomy–an apparently very common spinal surgery that residents typically perform and attendings simply oversee. I watched the surgery and noticed its tedious nature, cauterization and scraping away at the lamina over and over. The smell of burning flesh was ingrained in my mind. As I watched, I wasn’t sure how to feel–maybe neurosurgery wasn’t all that amazing like I expected.
Later that day however, a patient came in with a left frontal brain mass that needed to be biopsied. I was waiting for the surgery to begin when I saw this machine with two large screens being rolled into the OR. The machine had loaded up the imaging scans that they had taken of the patient’s brain a couple of days ago, and it had created a 3D image with the mass lit up in a bright blue. Before starting the surgery, the surgeon used this magic wand (it was really just a stick) to calibrate the machine in order to localize the mass and mark where to make her incisions. I jokingly asked the resident how surgeons performed a surgery like this in the past without the amazing technology and he laughed and said, “They really had to know their neuroanatomy!” The surgery began and I saw the process that it took to cut through the skin, drill through the skull, and finally remove the dura before getting to the beautiful brain. The surgeon walked me through every step and let me just stare at the brain for a few seconds. I was in awe! They localized the mass using the magic wand and I was able to observe how it was slightly different in color and texture from the rest of the brain tissue. They took a biopsy, sent it to the lab, and within a few minutes the lab called down to the OR indicating that it was a glioblastoma (a tumor that forms from the glial cells of the brain–turns out a lot of CNS and PNS tumors have pretty straightforward names like this one). Glioblastoma is a very aggressive cancer and the patient had multiple masses so the surgeon put on a microscope that played a live image on the OR screens and I watched as she tried to remove as much of the tumor as possible.
I went home that evening and I couldn’t wait to tell my parents everything that I saw. I shadowed in the clinic and the OR for another almost 90 hours that summer and witnessed some other pretty amazing surgeries, most notable were the awake deep brain stimulation surgeries for Parkinson’s disease, essential tremor, and facial pain; telling you about those would require a whole blog post in itself. At the end of the summer I could confidently say that neurosurgery turned out to be as exciting as I expected it to be.
RotaCare: A Mobile Clinic Helping the Uninsured
Written by: Gautam Naik | Edited by: Arshad Mohammed
I’ve spent the past semester and a half on UC Berkeley’s campus as a first-year undergraduate, and, as a premed student, I’ve made sure to explore many of Berkeley’s “clinical” opportunities. In my recent exploration, the work of mobile clinics became prominent and clearly foundational to the community. As such, I wanted to really understand the work of mobile clinics and how they look to improve the community, so I pounced on an opportunity to talk with a representative of RotaCare, a mobile clinic with 10 locations around the Bay Area, to understand more about the organization and their work.
- Just to start things off, I was wondering if you would be able to tell me a little bit about yourself and your connection with RotaCare?
I had the privilege of speaking with JP Sahi, who has been with RotaCare for the past 8 years and is currently Chief Executive Officer (and former Director of Clinic Operations) of the organization, being responsible for overseeing clinic operations and development. Before RotaCare, Ms. Sahi worked in numerous healthcare-related nonprofit organizations aligning with her passion of assisting people who do not have adequate access to healthcare. Her experience includes contributing to Federally Qualified Health Centers[1] like Bay Area Community Health[2] and Axis Community Health[3], just to name a few.
- How did the organization begin? What issues in the community became prevalent enough that they led to the formation of RotaCare?
RotaCare first began operations in 1989 in San Jose by Dr. Mark Campbell, who began to notice that a large portion of the community were left with inadequate access to healthcare. With the support of his Rotary Club, he helped establish the first clinic in Saint Agnes Hospital. Over time, the organization has grown and expanded, now being able to offer services in 10 different communities, including Santa Clara, Morgan Hill, Gilroy, and Richmond. With the help of volunteers, the Rotary community, and other donations, RotaCare has been able to provide free healthcare to members of their community unable to pay for primary healthcare.
- What kind of barriers does RotaCare help patients overcome when it comes to their access to healthcare and medical services?
RotaCare primarily provides assistance to the uninsured parts of the community. They help provide underserved communities with the necessary healthcare resources to live fruitful lives. That being said, their work extends beyond simply the uninsured. Through word-of-mouth, the services and assistance provided by RotaCare has become known throughout much of the community and are used by a wide array of people, all who face barriers to utilizing primary health care.
According to JP Sahi, a large, and not well-known, community that RotaCare serves is undocumented immigrants. Initially, many undocumented immigrants are hesitant to leave their homes in fear of deportation and are wary of the government’s help in regards to healthcare and other resources due to fear that their path to permanent residency and a green card could be hindered in some way. Personally, as a son of immigrant parents, I understand the importance of a green card and permanent residency in the US as it provides a sense of stability and security. In regards to the undocumented immigrants RotaCare assists, due to their apprehensiveness of the state and society as a whole, immigrants, undocumented and others alike, are unaware of the numerous healthcare services available at their disposal. They believe that spending more money on healthcare will invariably lead to better services and resources. However, this is not the case. RotaCare looks to bridge this gap through enrollment agents[4] and social workers[5] in order to help immigrants integrate into the healthcare system. Ultimately, residency status, language, and understanding the American healthcare system serve as major barriers to a patient’s ability to access healthcare and medical services.
- How does culture (i.e. Spanish speakers) affect patient’s healthcare access and how does RotaCare tackle this issue?
According to JP Sahi’s time in the healthcare industry, both with Rotacare and previously, language and culture serve as major barriers to communities gaining access to and utilizing the proper healthcare services and medical resources. Among the communities that RotaCare is involved in, the Spanish, Nepali, and Russian communities are those that face the largest cultural and language barriers in accessing healthcare resources. This predicament further increased during the COVID-19 pandemic, when many foreigners were stuck in the Bay Area due to travel restrictions. In addition to not being fully knowledgeable about the American healthcare system, language and culture barriers arose as these foreigners were predominantly Asian and particularly fluent in only their regional or national language, such as Punjabi, Hindi, or Mandarin. Then and now, RotaCare has looked to scale these barriers by recruiting volunteers who are able to bridge this divide as translators and provide patients’ with the correct resources. These volunteers help patients facing cultural and language barriers utilize the medical resources available along with providing a stress-free environment in which patients are able to make more informed decisions regarding their health.
- What type of services does RotaCare offer and how does it help contribute to the community?
RotaCare’s main objective is providing underserved parts of the community with the necessary medical services and healthcare resources in order to live healthy lives. As such, they help resolve any medical issue, and if the issue is beyond their resources, they will find referrals for their patients, which include the uninsured, undocumented immigrants, and people who face cultural barriers. They provide patients with access to free medical exams, diagnostic testing, lab testing, and many pharmaceuticals. Along with these services, RotaCare has an extensive program that educates the community in diabetes and hypertension and is currently running a pilot program funded by John Muir regarding these health conditions. RotaCare also helps educate the community on best health practices, healthy eating, proper exercising, and how to shop smartly for the best foods. RotaCare not only provides the community with medical services that help resolve any existing health issues but also improves the general health awareness of society in a bid to prevent these health concerns from ever arising.
- From your time and experience with RotaCare, how has RotaCare impacted the lives of the people it serves?
During her time at RotaCare, JP Sahi has personally seen the impact that its services have had on the people it assists. RotaCare provides an avenue from which underserved parts of the community are able to inquire about what seems to be minor issues in their health. However, these issues can often be early signs of larger, more complicated problems, like cancer. Ms. Sahi has seen patients be able to use RotaCare’s services to investigate smaller issues in their health and, as a result, prevent larger issues from arising later in life. During our conversation, she gave an example of a patient who met a RotaCare provider at an outside event some time after his first visit to the organization. This patient had first visited their local RotaCare clinic after reporting abnormally high blood pressure levels. After being triaged, the patient was sent to the ER in order to have more thorough tests done. After the results were analyzed, it was learned that the patient suffered from a critical condition that had life-threatening consequences. However, since it was detected very early on, any major consequences were avoided. It is this type of service that RotaCare seeks to provide and the type of impact it has had on the communities it serves.
- How can the community get involved in this initiative?
RotaCare does not stand alone in its efforts to improve healthcare access and services for all people in the community. Along with a vast array of other organizations, RotaCare seeks to help people live more comfortable lives and be more knowledgeable about their own health. In my conversation with JP Sahi, she stressed the rising need for additional mental health services along with educating the community on existing resources. In a world centered around social media and post-pandemic recovery, mental health is of crucial importance and must be properly protected and nurtured in order to ensure a healthy community.
Right now, as a community, we can work towards RotaCare’s vision by raising awareness about available medical and mental health services. We can help support these non-profit organizations through fundraisers and by becoming certified healthcare workers. By volunteering at organizations like RotaCare, we can help improve the general welfare of our community. Even simply being more knowledgeable about healthcare and about local medical and mental health resources can go a long way in ensuring that the people in our community get the help they need when they need it.
______________________________________________________________________________
- Federally Qualified Health Centers: Community-based organizations that provide a variety of primary and preventive care services to people regardless of their income or health-insurance status.
- Bay Area Community Health: Provide health and social services with the goal of providing everyone in a community with equal access to high quality and affordable healthcare in Alameda and Santa Clara County
- Axis Community Health: Promotes the wellbeing of members in the community, especially those struggling from poverty, housing instability, and social disparities, across Eastern Alameda County by offering affordable and accessible health care services.
- Enrollment Agents: Work alongside social workers to ensure that immigrants are able to gain access and navigate through the US healthcare system.
- Social Workers: Supports individuals and families by ensuring people gain or utilize access to basic necessities such as food, shelter, and healthcare. Their ultimate goal is to improve the social environment and welfare of people.
Anki: A Word of Warning and Fundamental Guide
Written by: Angelic Cox | Edited by: Arshad Mohammed
You arrive on test day, forgetting the small details your biology class began testing you on. This builds anxiety within you, and your fear of not understanding how to get to the correct answer leads to lower exam performance.
Fortunately, there is a solution to your problem. Through Anki, digital flashcard creation can help you remember specific facts presented throughout your course.
Before we start on the technicalities of flashcard creation, here is a warning: Anki should be used for lower-order thinking skills(lower-order processing) of specific details that cannot be integrated into a concept. You can test if something is a detail if it relies on abstract words and cannot be translated into an image. For example, in my ESPM 50 AC course, a small detail I believed was important was “Indians perceived transaction as an agreement between 2 sovereign groups, English thought it was economic transaction under English law”(Cronon,8). It is difficult to rely on an image to exemplify the abstract concept of economic transaction under English law and 2 sovereign groups, so words and memorization are needed in this process.
I also want to emphasize that lower-order processing should not be the primary learning technique you rely on– which is a mistake many students and I have made. If you end up with thousands of flashcards for a 15-week course, you are studying wrong.
Your primary learning techniques should rely on high-order processing skills, which can be applied intuitively during listening and reading. This will lead to a more succinct note-taking and analysis process. I plan to cover high-order learning skills in another article, such as mind map creation.
1: the levels of higher-order thinking skills and lower-order thinking skills
Lower-order thinking skills – bloom’s taxonomy. Google Sites: Sign-in. (n.d.) from https://sites.google.com/site/supersophomores675/l
Since we know that flashcards are a secondary study technique, we can move on to the creation side.
How do flashcards work?
Flashcards rely on spaced repetition, which is when you leave a topic for some time and then come back to it to revise. The intervals of time you leave in between is up to you, but I suggest doing at least a few cards daily so you are constantly being exposed to the material you want to memorize.
How do I get started with Anki?
1. Go to AnkiWeb and download the software on a personal computer. There are mobile versions, but on iOS, it costs around $25.
2. Open Anki and hit “Create Deck,” where you will name the deck.
3. Open the deck you just created and press “Add” to start your flashcard creation
How do I make flashcards on Anki?
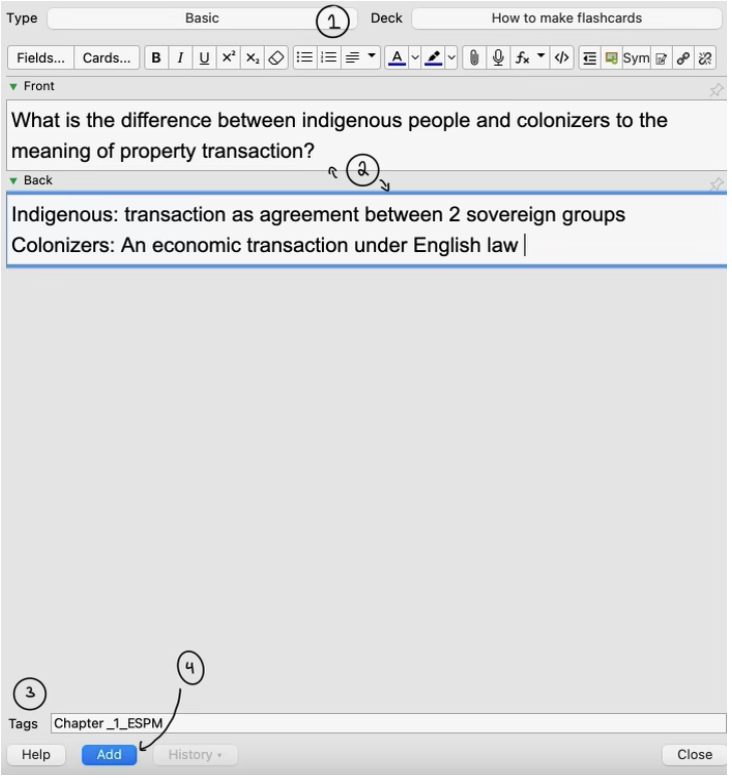
- When starting, you should stick with the “basic” card type. But there are other card types available that you can download online. Another popular card type to use is “cloze deletion”. You can look into it, but it is not necessary to use.
- You type your question relating to the material within the “front” text box and your answer in the “back” text box.
2.1 Here is a resource on the creation of questions for flashcards.
- Tags can help group your flashcards, so I recommend adding a tag.
3.1. You can create “subdecks,” but it should be done rarely. Having tags in your organization system is better since it is less cluttered.
- Add your cards, and you can begin studying!

- The buttons at the bottom of the screen are a way to gauge how well you memorized the material. You can self-judge how well you know the fact, but as a general guide, most of your cards should be in the “Good” section, some in the “Hard” and “Easy” sections, and little within the “Again” section.
- You must learn the material beforehand, so if you consistently press “Again,” you must engage in higher-order processing.
- The times on the top of the buttons are when you need to come back and revise the flashcards. They are the interleaving intervals.
- You must revise your cards daily to benefit from the spaced repetition method.
It may feel uncomfortable when you begin to change your study methods because you are thinking in an unconventional way to you. Just know that this discomfort means that you are learning. As a result, you will have a more efficient study process.
Next time you walk into a test, you won’t be thrown off by the small details presented.
Our Responsibility as Advocates and Healthcare Professionals
Written by: James Kim | Edited by: Arshad Mohammed
The summer before my junior year, I volunteered to become an adaptive sports instructor for the non-profit Achieve Tahoe. Ever since I was 4 years old, my grandfather had taught me both alpine and water skiing – memories of which I still find extremely nostalgic. Thus, I came with a passion to share my love for outdoor sports, but more importantly, a passion to create the same fun and exciting experiences I had with my grandfather for others.
One of my favorite participants I worked with that summer was a 6-year old named “Emily.” Emily always came early for her lessons, and she always had the biggest smile and the cutest squeals of joy as she looked towards the lake and got excited to waterski. However, over the course of 3 different days and 3 different lessons, she was never really able to get the “balance” of waterskiing. I would try to teach her through all sorts of different options – having her hold onto different ropes, different hand positions, having someone on the boat try and tell her the directions as she water-skied, etc. It seemed like no matter what I did, however, I just could not convey the proper technique she needed to waterski. After the end of the 3rd day, I could only think about how I failed as mentor and as teacher. I asked myself – what could I do differently to help her succeed in the future?
As I was taking part of the end-of-day staff meeting, Emily’s mother came up to our group and thanked us all for our hard work. She said that she never even thought that Emily would want to go into the water, nonetheless be excited to try waterskiing every day. Despite the three days of what I would have previously called “failures,” her mother noted that Emily always came back home with a great smile. She would beg her mother to try more water-skiing since it was “berry berry fun,” to her.
When I think about this experience in hindsight, I learned a key lesson that success means something different for everyone. What one deems to be a significant accomplishment is different than what another deems to be so. But with that being said, as an advocate for others, we then have the responsibility to not also project our own feelings of what is “success” especially when thinking about others and their goals and motivations.
As future healthcare professionals and leaders in medicine, I believe that it is important for us to provide re-affirming and patient-centered care. To me, this means recognizing the needs and goals of individuals and their particular lifestyles, and how I could create an environment people my patiens feel like they could succeed and achieve their goals in spite of their healthcare issues. So now I ask – what does this mean for you?
To Operate, or to Not Operate
Written by: Arshad Mohammed | Edited by: James Kim
Over the summer, I had the pleasure to shadow surgeons at an overseas hospital. After seeing life-altering procedures and the intricate details of human anatomy up close, this experience has solidified my desire to become a surgeon.
Surgeons have the privilege to correct and treat structural issues, and oftentimes they can provide immediate relief. People are trusting you with their lives, and you have to reassure them in a time of great emotional distress. Being confident and making patients feel comfortable during the entire process is a crucial skill. The intimate nature of this patient-doctor relationship means you are there during the lowest of lows or the highest of highs.
However, during my experience, I soon learned that a great surgeon also knows when to operate and when not to. My mentor, an orthopedic surgeon, would always explain to his patients in the clinic that surgery is a last resort. Surgery should only be considered when the symptoms of your conditions make everyday life difficult and your quality of life plummets. The potential benefits should always outweigh the risks.
This was exemplified when my mentor saw a patient with a broken arm in his clinic. This middle-aged patient came in with his mother. The patient felt a screw pop out of a metal plate in his arm a few days prior. Further inspection confirmed this, and he required surgery. The patient explained he was a police officer who needed to go on duty and he couldn’t afford another surgery on his arm. Over 2 years, he had undergone 5 surgeries because of complications with infections and screw placement.
His arm was so weak he could not lift a water bottle. As he recounted the car accident that gave him this broken arm, his mother started weeping. She sobbed and said, “my son was as strong as an ox. Now he is a cripple. Can’t you do anything?”. Dr. X weighed both options and let the patient decide. He chose to forgo the surgery.
As healthcare professionals, we need to consider the wellness of the patient as a whole. We can’t make tough decisions on their behalf. Sometimes, preserving the quality of life is more important than treating illness. This humanistic side of medicine is what drives me to be a physician.
Written by: Christine Wan | Edited by: Zainab Bhatti and Nicole Xu
Importance of Blood Donations
Annually, roughly 6.8 million people in the United States donate blood and 4.5 million patients will require a blood transfusion. Because blood cannot be synthetically produced in laboratories, there are no synthetic substitutes. As a result, certain patients are dependent on blood donations for their survival. For instance, cancer patients are in constant need of blood due to many reasons including: blood loss during surgery, low blood cell count due to the side effects of chemotherapy and radiation, or anemia. Cancers of the blood and bone marrow, such as leukemia and lymphoma, are another reason transfusions are required because the disease does not allow the body to produce normal blood-making cells (Rodriguez). Other patients who require blood transfusions include: women who experience ectopic pregnancies, women who hemorrhage at any stage of childbirth, children with severe anemia often resulting from malaria or malnutrition, people with severe trauma due to man-made and natural disasters, and patients with thalassemia, hemophilia, and sickle cell disease (WHO).
Today, most medical care centers and hospitals are dependent on a steady supply of blood from donors since one in seven people entering the hospital need blood. For centers treating cancer patients, this steady blood supply is especially important because as cancer care increases, the demand for blood and platelet donations increases as well. An adequate amount of blood is needed in all health care facilities for patients facing trauma and other lifesaving procedures. As such, blood transfusions and donations are able to aid in saving millions of lives each year (Rodriguez). Additionally, there is a constant need for a regular blood supply because it can only be stored for a limited time before use. Regular blood donations by a sufficient number of healthy people are needed consistently to ensure that safe blood will always be available when needed to best treat patients and offer them the best chances at recovery (WHO).
Moreover, there are several types of blood donations and one donor can help up to three patients. A single unit of blood can be separated into different components: red blood cells, plasma, and platelets. “Whole blood” is the most common and most flexible blood donation. It is usually collected in one pint and separated into different components in order used to help multiple patients. Plasma is collected through apheresis- a process that separates plasma from other blood components. It has blood clotting factors needed to help trauma patients and those battling certain diseases like cancer. Platelets are also collected through the apheresis process. Once platelets have been selected from the donor’s blood, the red blood cells and other fluids are returned to the donor. Cancer patients are the primary recipients of platelets as they play an important role in cancer treatment. “Double red cell” donation is the collection of only red cells through the apheresis process. It allows donors to give double the amount of a “whole blood” donation and can be used for anyone suffering from blood loss (Rodriguez).
Overall, blood donations and a steady supply of blood are requisite to the survival of so many patients. Donating blood even once can be utilized to aid in the recovery of several patients.
Bibliography
Rodriguez, Jonesa. “The Importance of Blood Donations.” Moffitt Cancer Center, 13 May 2020, moffitt.org/endeavor/archive/the-importance-of-blood-donations/.
WHO (World Health Organization). “Blood Products: Why Should I Donate Blood?” World Health Organization, World Health Organization, 13 June 2017, www.who.int/news-room/q-a-detail/blood-products-why-should-i-donate-blood.

Written by: Arathi Vinod | Edited by: Sameer Rajesh and Nicole Xu
Stress During COVID-19
Stress is difficult enough to manage without a global pandemic.
The COVID-19 pandemic has left its unpleasant mark on everyone’s lives in one way or another. Whether this involves coping with the loss of a loved one or putting up with an ever-changing lifestyle, COVID-19 has caused a global change in the way civilization fundamentally functions. Therefore, it should come as no surprise that the pandemic has greatly increased stress worldwide.
Despite the negative context with which it is often used, stress is a natural, and even beneficial, biological process. Commonly known as the “fight-or-flight” response, stress is an evolutionarily clever development that helped early organisms escape immediate danger.
Any life-threatening event triggers the sympathetic pathway of the body’s autonomic system. Tissues receive sensory input and transfer this information to the central nervous system via neurons. Finger-like dendrites of a preganglionic neuron then take in this information and transmit it as electrical signals across its axon through an action potential (Brown). As the action potential reaches the neuron’s synapse, it releases vesicles filled with the neurotransmitter acetylcholine. These small chemical substances diffuse to the dendrites of another neuron, where they bind to nicotinic acetylcholine receptors (Brown). Just like the first neuron, this postganglionic neuron goes on to transmit this information along its axon and eventually releases another neurotransmitter called norepinephrine. Norepinephrine molecules finally bind to muscarinic acetylcholine receptors on smooth or cardiac muscles and ultimately bring about the changes associated with stress (Brown).
The sympathetic pathway generates a variety of stress responses in the body. For instance, a common characteristic of the fight-or-flight response is increased heart rate (“Understanding the Stress Response”). Similarly, a sympathetic response can trigger pupil dilation, bronchial dilation, and digestion inhibition (“Understanding the Stress Response”). These reactions help the individual escape the instantaneous threat by prioritizing increased environmental assessment and oxygen intake while giving less importance to other bodily processes.
However, COVID-19 is no instantaneous threat. The global outbreak has persisted for over a year now, and individuals’ increased health concerns and turbulent lifestyles have led to a more long-term stress response. Chronic stress repeatedly triggers the same sympathetic pathways, and this can have a severe, irreversible impact on the body. For example, a persistent increase in heart rate can lead to cardiovascular strain, increasing the risk of hypertension and heart disease (“Understanding the Stress Response”). Likewise, along with digestion, the body also inhibits the immune system while stressed. Therefore, overtime, the body becomes less capable of defending itself against infections (“Understanding the Stress Response”).
Fortunately, stress is curable, and the cure does not have to involve medication. Exercise and meditation not only serve as diversions from stress factors, but they also release endorphins, the body’s natural morphine that stimulates a sense of positivity (“Physical Activity Reduces Stress”). Diet is also critical; healthy eating can reinvigorate the immune system and counteract the negative effects of chronic stress. Additionally, just as exercise increases desirable hormones, caffeine acts as a stimulant, increasing the amount of stress hormone cortisol in the body, and should be avoided (Scott).
Of most importance is the understanding that no one is alone in this struggle. COVID-19 might have overstayed its welcome, but stress does not have to.
Bibliography
Brown, Jacquelyn. “Fight or Flight: All You Need to Know About This Response.” CogniFit, 16 May 2017, blog.cognifit.com/fight-or-flight/.
“Physical Activity Reduces Stress.” Anxiety and Depression Association of America, ADAA, ADAA, 2019, adaa.org/understanding-anxiety/related-illnesses/other-related-conditions/stress/physical-activity-reduces-st.
Scott, Elizabeth. “How Does Caffeine Affect Your Stress Levels?” Verywell Mind, 17 Jan. 2020, www.verywellmind.com/caffeine-stress-and-your-health-3145078.
“Understanding the Stress Response.” Harvard Health Publishing, Harvard University, Mar. 2011, www.health.harvard.edu/staying-healthy/understanding-the-stress-response.

Written by: Zeynep Demirag | Edited by: Zainab Bhatti and Nicole Xu
Understanding Clinical Trials
The clinical trial process is how a medical intervention such as a drug, device, or procedure moves from an idea to patient care (Mayo Clinic). Clinical trials are research studies that evaluate new ways to improve treatments and quality of life for people with diseases such as pancreatic cancer. Clinical trials are an option for all patients to consider and play an important role in improving health care. Results from clinical trials help develop new drugs, diagnostic tools, and clinical procedures. They can also evoke a new question for research which can lead to new discoveries over time and help us better understand diseases. All the drugs and medical devices used today were approved for use because patients volunteered for clinical trials.
Every clinical trial has “eligibility criteria” where a patient may need to have a certain medical condition, gender, or other specific quality to meet participation criteria (NIH). According to the beneficence principle of The Belmont Report, patients who want to volunteer need to understand potential benefits and risks (OHRP). Patients may personally benefit from receiving new treatments, therapies, or procedures. They also receive close supervision from clinical staff. On the other hand, patients might risk not benefitting from the new treatment and devoting a large amount of time to participate in a clinical trial. Informed consent is a process that helps patients to make a decision to consent whether to join a clinical trial or not. An informed consent document is provided and explains the purpose, procedures, potential benefits, and risks of the trial.
There are four different phases of clinical trials in which safety is emphasized. If a trial does not have a healthy and safe outcome at any phase, then it will not be allowed to proceed to the next trial phase. Before phase I begins, there is phase 0 where the new treatment has already been found to be safe in animals or healthy human volunteers (NIH). Phase I trials are designed to find the safe dose of treatment, determine how the treatment should be given, and learn how it affects the body. Phase I trials can last several months and approximately 70% of the new drugs move to the next phase (FDA). If a safe dose is found, the new treatment goes to phase II testing. Phase II is conducted with a larger patient group than the previous phase — usually having up to several hundred people. This phase studies how well a treatment or combination of treatments works for a certain type of disease. The length of Phase II can be anywhere from several months to two years, and 33% of drugs usually move to the next phase (FDA). At phase II, the eligibility criteria becomes more restrictive, and phase II studies can be either randomized or nonrandomized. If a new treatment is found to be safe and have benefits, it proceeds to phase III. Phase III trials are conducted in an even larger group of participants, and the length for Phase III can be anywhere from 1 year to 4 years. Approximately 25%-30% of drugs move to the next phase (FDA). Phase III involves a randomized design comparing the new treatment to the standard treatment. If a phase III clinical trial is positive, the new treatment will be approved and licensed for use in the US by the FDA. After the treatment is approved, phase IV clinical trials involve monitoring to continue assessing safety effectiveness, and optimal use.
Clinical trials play an important role in moving science forward and can be a hopeful option for many patients with certain diseases (NIH).
Bibliography:
Office for Human Research Protections (OHRP), OHRP. “Read the Belmont Report.” HHS.gov, US Department of Health and Human Services, 15 Jan. 2018, www.hhs.gov/ohrp/regulations-and-policy/belmont-report/read-the-belmont-report/index.html#:~:text=Beneficence.,to%20secure%20their%20well%2Dbeing.
Commissioner, Office of the. “Step 3: Clinical Research.” U.S. Food and Drug Administration, FDA, www.fda.gov/patients/drug-development-process/step-3-clinical-research.
NIH National Institute on Aging (NIA). “What Are Clinical Trials and Studies?” National Institute on Aging, U.S. Department of Health and Human Services, 2020, www.nia.nih.gov/health/what-are-clinical-trials-and-studies.
Mayo Clinic, “Clinical Trials – About Clinical Studies.” Mayo Clinic, 25 Feb. 2020, www.mayo.edu/research/clinical-trials/about-clinical-studies.

Written by Athira Vinod | Edited by: Sameer Rajesh and Nicole Xu
The Basics of Long Term Care
Although people depend on guidance from others at every stage of their lives, care means the most when one becomes unable to tend to themselves. Long term care, also referred to as LTC, encompasses every form of care necessary to support individuals who are incapable of caring for themselves as a result of disability or illness. Considering the increase in chronic illnesses and a general decline in health as one ages, long term care is most commonly a division of care reserved for the elderly population; since diseases like dementia make it impossible to live independently, older individuals require additional assistance for long periods of time.
Although nursing homes are a well known component of long term care, it can also include home care, adult day health care, and assisted living. As the name suggests, home care allows for the individual to remain at home while being cared for (American Council on Aging). Home care aides assist in both daily maintenance activities, such as feeding, dressing, and using the restroom, and instrumental activities of daily living (IADLs) that are not as essential but still necessary to live satisfactorily, such as doing the laundry, buying groceries, and making meals (American Council on Aging). Adult day health care is a component of long term care that may be most attractive to families in which caretakers have other duties that prevent them from providing maximal care for elderly members. Available for part of the day, adult day health care is an option that offers individuals a community environment and basic medical services while family is away for work or other responsibilities. Elderly people can also opt for assisted living. A less intensive version of nursing homes, assisted living involves personal assistance, housekeeping, and recreation without 24-hour care (American Council on Aging). Because those who receive this form of care do not necessarily need as much assistance as others with more severe illnesses, assisted living may or may not be considered a form of long term care, depending on the particular level of care involved (American Council on Aging). Other than these major categories, long term care can also be adapted to fit the specific illness an individual is facing, such as the use of memory care for Alzheimer’s patients.
Because long term care focuses on one of the more vulnerable populations in our society, consistent revision and improvement are necessary to ensure the best quality of living for those involved. For instance, the reduction in elderly individuals’ autonomy following the transition to long term care is one area that has been under scrutiny. In response, the idea of “culture change” has emerged as a potential solution (Pioneer Network). The culture change movement has pushed for the emphasis of choice in long term care, resulting in the elderly feeling more respected, more comfortable with the assistants they associate with, and happier in their new environments (Pioneer Network). For many long term care facilities, the lack of resources has also made it difficult to promote staff education (Silvestre, et al.). In an attempt to circumvent financial barriers, facilities have begun several initiatives that keep staff well-informed through less expensive methods. Online programs, staff presentations, and recognition for overachieving employees have all played a role in increasing awareness and encouraging education without spending too much money (Silvestre, et al.). Implementing such changes and staying aware of what the elderly need most can help keep long term care facilities safe and happy environments for the people they are meant to protect.
Bibliography
American Council on Aging. What Defines Long Term Care? 28 July 2020, www.medicaidplanningassistance.org/what-defines-long-term-care/.
Pioneer Network. Defining Culture Change. 4 May 2017, www.pioneernetwork.net/culture-change/what-is-culture-change/.
Silvestre, Josephine H., et al. “Improving the Quality of Long-Term Care.” Journal of Nursing Regulation, vol. 6, no. 2, 2015, pp. 52–56., doi:10.1016/s2155-8256(15)30389-6.

Written by: Christine Wan | Edited by: Zainab Bhatti and Nicole Xu
The Pandemic Diet
Since the start of quarantine, people have found themselves increasingly bored. This state is often associated with a greater energy intake and greater consumption of fats, carbohydrates, and proteins (Muscogiuri et al.). The increased stress associated with quarantine pushes many people to overeat and look towards sugary “comfort foods.” This desire to consume a specific kind of food is defined as a “food craving.” Food cravings involve a broad range of processes including those in the emotional, behavioral, cognitive, and physiological domains.
In particular, craving carbohydrates is associated with increased serotonin production which has positive impacts on a person’s mood. As such, carbohydrate-rich diets could be utilized as a form of self-medicating against stress (Muscogiuri et al.). However, carbohydrate craving is a relatively unhealthy nutritional habit, holding the potential to increase the risk of developing obesity. Obesity stands as a serious medical condition, given that it is associated with chronic inflammation as well as complications related to heart disease, diabetes, and lung disease. Furthermore, all of these conditions have been demonstrated to increase the risk for more serious complications of COVID-19 (Muscogiuri et al.).
Stress resulting from quarantine has also led to sleep disturbances, which positively reinforce the worsening of stress and increased food intake (Muscogiuri et al.). As such, a dangerously vicious cycle emerges. Thus, it is important to consume food containing or promoting the synthesis of serotonin and melatonin during meals, especially dinner.
A large variety of plant species, like roots, leaves, fruits, and seeds, contain melatonin. Specific foods include almonds, bananas, cherries, and oats. All of these may also contain tryptophan- a precursor of melatonin. Protein foods, such as milk and milk products, on the other hand, are the main sources of this sleep-inducing amino acid. Moreover, beyond sleep-inducing properties, milk products can also augment natural killer cell activity and reduce the risk of respiratory infections (Muscogiuri et al.). In other words, these products are able to strengthen the immune system and the immune response.
Other dietary advice includes some information disseminated by the World Health Organization (WHO). A bulk of this information includes limiting salt, fat, and sugar intake as well as increasing consumption of fiber and plant species-echoing the statements referenced above. The WHO also indicates the importance of staying hydrated, limiting alcohol consumption, prioritizing fresh ingredients, making home-cooked meals, taking advantage of food-delivery services, and enjoying family meals. The organization also recommends cooking food thoroughly as well as keeping all utensils and kitchen areas clean (World Health Organization). Additionally, the WHO recommends purchasing long-lasting fruits and vegetables, whole grains, starchy roots, eggs, general milk products, and reduced-fat, shelf-stable milk.
Overall, quarantine and its related aspects have caused nutrition to become a larger priority. From ensuring certain foods are included in our diets to limiting our intake of certain foods, our diets have become increasingly important as a means to decrease and keep negative health effects at bay.
Bibliography
Muscogiuri, Giovanna et al. “Nutritional recommendations for CoVID-19 quarantine.” European
journal of clinical nutrition vol. 74,6 (2020): 850-851. doi:10.1038/s41430-020-0635-2.
World Health Organization (WHO). “Food and Nutrition Tips during Self-Quarantine.” World
Health Organization, 2019, https://www.euro.who.int/en/health-topics/health-emergencies/coronavirus-covid-19/publications-and-technical-guidance/food-and-nutrition-tips-during-self-quarantine. Accessed 7 Feb. 2021.

Written by: Arathi Vinod | Edited by: Sameer Rajesh and Nicole Xu
The Ethics of Animal Testing
From developing vaccines to ensuring acceptable health standards for household products, there is one step in the scientific testing process that is as vital as it is controversial: animal testing. Animal testing is not a new thing; using animals for the sake of medical research has been around since the time of ancient Greek philosophers and scientists (Hajar). However, a deeper analysis into the flaws and benefits of animal testing did not occur until quite recently. With an overall rise in humanitarian efforts like women’s rights and anti-slavery movements, the 1800s also spurred on movements against animal cruelty, leading to the rise of organizations like SPCA in England and America (Walls). On the other hand, recent events have also highlighted the other side of the debate on animal testing. In 1937, a medication called Elixir Sulfanilamide caused over one hundred deaths due to a toxic solvent used in it called diethylene glycol (DEG). Having done no animal testing before selling the drug, pharceutical companies were forced to face the angry public, and the Federal Food, Drug, and Cosmetic Act was promptly passed, mandating animal testing on drugs to ensure safety for human usage (Hajar). Today, there are still two distinct sides to the animal testing debate, and it is worth exploring the principle arguments of both.
Downsides of Animal Testing
When discussing the topic of animal testing, perhaps the most evident downside is the cruelty with which animals are treated in medical labs. Common lab procedures include surgically interfering with the biological systems of animals, knocking down particular genes to see their effects on the animal, and injecting or otherwise exposing animals to chemicals that can physiologically harm them. Even for research methods that do not require direct harm on the animals, procedures like forcefully restraining animals and clipping their tails for identification purposes cause physiological and psychological pain for the animals being tested on (“About Animal Testing”). By regarding human life as more worthy of protecting and morally superior to animal life, experimenters are arguably displaying speciesism, or prejudice against nonhuman species (Liou).
Those against animal testing point out that not all drugs that go through animal testing produce safe results for humans. For instance, in addition to the poisonous DEG-containing Elixir Sulfanilamide, another drug that incited more emphasis on animal testing was thalidomide, a painkiller drug of the 1960s that caused deformities in children of pregnant users (Hajar). Upon insistence from the outraged public, thalidomide was tested on pregnant animals to observe the results. However, surprisingly, it was found that the offspring of these animals were not affected in the same way human children were (Greek et al.). Thus, animal testing is not always as effective as it is often made out to be.
Benefits of Animal Testing
Supporters of animal testing primarily argue that the advantages for humans far outweigh the disadvantages for animals being tested on. In opposition to the speciesism argument of animal rights activists, those who defend animal testing claim that humans and animals cannot be considered on the same moral ground. The reason for this is that nonhuman species do not practice autonomy and independent judgment like humans do. Therefore, from a philosophical perspective, testing on animals cannot be perceived with the same lens as testing on humans because humans and animals do not belong in the same moral community (Liou). Furthermore, so many of the last centuries’ most remarkable medical advancements were made possible due to animal testing. The medical field owes animal research for significant developments such as anesthetics, the polio vaccine, and antibiotics (Fisher). These momentous breakthroughs in medicine put into perspective the vast impact that animal research has had on human civilization.
Animal testing advocates go on to note that the disadvantages of animal testing are outweighed not only by the advantages to humans, but also the advantages to other animals. The medical cures and treatment techniques derived from animal research are not limited to human use, and many animal-tested remedies have been beneficial to animals. For example, Siberian polecats were used to test the efficacy and safety of the distemper vaccine, but this vaccine proved vital in saving the black-footed ferret from extinction (“Animal Research”). Such instances are not uncommon, and many dwindling animal populations have been rescued from potential extinction through treatments that ultimately utilized animal testing techniques.
The debate still stands as to whether testing on animals is worth the cruelty it imposes. In the meantime, several alternative methods that minimize animal usage are being looked into, including computer models that simulate human biology, in vitro cell screenings, and stricter regulations mandating humane treatment of animals in research labs (“About Animal Testing”).
Bibliography
“About Animal Testing.” Humane Society International, 27 May 2020, www.hsi.org/news-media/about/.
“Animal Research.” American Association for Laboratory Animal Science, AALAS, 2020, www.aalas.org/public-outreach/animal-research-faq.
Fisher, Elizabeth. “Why We Should Accept Animal Testing.” Huffington Post, 17 July 2013, www.huffingtonpost.co.uk/professor-elizabeth-fisher/why-we-should-accept-anim_b_3608923.html.
Greek, Ray, et al. “The History and Implications of Testing Thalidomide on Animals.” The Journal of Philosophy, Science & Law, vol. 11, no. 3, 2011, pp. 1–32., doi:10.5840/jpsl20111133.
Hajar, Rachel. “Animal Testing and Medicine.” Heart Views, vol. 12, no. 1, 2011, p. 42., doi:10.4103/1995-705x.81548.
Liou, Stephanie. “The Ethics of Animal Experimentation.” HOPES Huntington’s Disease Information, Stanford University, 26 July 2017, hopes.stanford.edu/animal-research/.
Walls, David. “Animal Rights Movement.” Sonoma State University, 2015, web.sonoma.edu/users/w/wallsd/animal-rights-movement.shtml.

Written by: Zeynep Demirag | Edited by: Zainab Bhatti and Nicole Xu
COVID-19 Vaccines: Moderna vs. Pfizer-BioNTech
Researchers currently have 67 vaccines under clinical trials, in which 20 of them have made it to the last step to be considered safe in humans. The different types of vaccines effective against COVID-19 include mRNA, protein, and inactivated vaccines. Although protein and inactivated vaccines are effective and approved in other countries, Pfizer-BioNTech and Moderna are currently the only two vaccines that have passed clinical trials and have been approved in the US. These two vaccines are similar in terms of technology and time-line, but they also differ in certain ways.
Moderna and Pfizer-BioNTech vaccines are both mRNA vaccines, which is a technology used to protect against COVID-19 infectious disease and to trigger an immune response. mRNA vaccines do not put a weakened or inactivated pathogen into our bodies like other COVID-19 vaccines approved in other countries. Rather, mRNA vaccines encode proteins that are then manufactured by the cells to make a protein, or peptide, to trigger an immune response (National Center for Immunization and Respiratory Diseases). Moreover, both Pfizer-BioNTech and Moderna vaccines are two doses. The Moderna vaccine comes in two separate 100 microgram doses that are given 28 days apart, while the Pfizer-BioNTech vaccine comes in two doses of 30 micrograms given 21 days apart. Moderna vaccines showed 94.1% efficacy rate and Pfizer-BioNTech vaccine showed 95% efficacy rate in a 38,000-person trial.
In terms of differences, the Pfizer-BioNtech vaccine had a clinical trial with younger people aged 16 and older. Consequently, their vaccines are approved for 16-year olds and older. The Moderna vaccine, on the other hand, had a clinical trial with participants aged 18 years and older, so Moderna vaccines have been approved for people aged 18-years and older. Moreover, storage protocol for the two vaccines differ. Pfizer-BioNTech vaccines are stored at -94 degrees Fahrenheit, while Moderna vaccines are stored at -4 degrees Fahrenheit. Thus, Moderna vaccines can be stored in a home freezer for 30 days, while Pfizer-BioNTech vaccines can be kept in a home freezer for only 5 days before they expire. The last difference between these two vaccines is that Pfizer-BioNTech developed the vaccine independently, while Moderna developed it in partnership with the National Institutes of Health (Anderson).
There is no current evidence that mRNA vaccines cause or intensify autoimmune disease (Diamond). Lastly, both of these vaccines will not be affecting the DNA of your cells or cause your immune system to attack your own cells. These vaccines are going to protect you from coronavirus by entering your system. Though long term side effects of mRNA vaccines are theoretical. Furthering this point, Betty Diamond, an immunologist and rheumatologist at the Feinstein Institutes for Medical Research of Northwell Health, states that: “At the moment there’s every reason to suggest that people with autoimmune diseases ought to get either of these vaccines when they get rolled out” (Diamond). Overall, COVID-19 vaccination will be an essential tool to prevent the spread of the virus and to help stop the pandemic; therefore, everyone with or without underlying condition will have the best protection against the COVID-19 infectious disease.
Bibliography:
National Center for Immunization and Respiratory Diseases (NCIRD). “Understanding MRNA COVID-19 Vaccines.” Centers for Disease Control and Prevention, 18 December 2020, www.cdc.gov/coronavirus/2019-ncov/vaccines/different-vaccines/mrna.html#:~:text=mRNA%20vaccines%20are%20a%20new,that%20triggers%20an%20immune%20response.
Anderson, Maia. “Pfizer-BioNTech vs Moderna Vaccines.” Becker’s Hospital Review, 28 December 2020, https://www.beckershospitalreview.com/pharmacy/pfizer-vs-moderna-covid-19-vaccine-what-s-the-same-what-s-different.html
Diamond, Betty. “COVID-19 Vaccine FAQ: Safety, Side Effects, Efficacy.” WebMD, 22 January 2021, www.webmd.com/vaccines/covid-19-vaccine/news/20201217/covid-19-vaccine-faq-safety-side-effects-efficacy#:~:text=Betty%20Diamond%2C%20MD%2C%20an%20immunologist,for%20people%20with%20such%20conditions.

Written by Athira Vinod | Edited by Sameer Rajesh and Nicole Xu
Organ Donation: How to Make a Bigger Difference
Ever since the first kidney transplant in the 1950’s, organ transplants have gained popularity as a potential solution to many of the most devastating illnesses. Whether the transplant is with principal organs, such as the heart, kidney, or lungs, or with more minor organs, such as skin or bone marrow, the use of organs from another individual has saved many lives.
Organ donation generally falls under two main categories: those from living organ donors and those from cadaveric organ donors (University of Minnesota). Living donors are able to donate organs in cases where the removal does not harm the donor. Procedures that take one in a set of organs, as with the kidney, or part of an otherwise functional organ, as with the lung, are both viable options for living donors (University of Minnesota). Cadaveric organ donation occurs after the donor has died. In this case, the decision to give an organ is made either by the donor before their death or by their family after their death, depending on specific state legislation. The distribution of the organs is determined by the United Network for Organ Sharing (UNOS), which holds a waiting list of patients looking for organ donations (University of Minnesota). After verification of factors including organ size, blood type, and location of the donor in relation to the patient, the organ is finally sent to a transplant center where the patient can receive the organ (University of Minnesota).
Despite the incredible impact organ donations could have, the numbers have failed to satisfy demands. There are several potential reasons for the steadily rising numbers of patients on donation waiting lists and a comparatively stagnant slope of donors. The increase in people seeking donated organs can be explained in part by the large elderly population, which results in a rising need to replace failing organs (“Organ Transplantation”). The advancement of technology has also played a role in increasing organ demand by making it possible to execute more complex medical procedures (“Organ Transplantation”). Unfortunately, the expanding need for organs is not matched by the donor count. Although more than 100,000 patients per year need organ transplants, only about 40,000 procedures are carried out (Health Resources and Services Administration). A new patient is added onto the waiting list every 9 minutes, and 17 people die every day from lack of an organ transplant (Health Resources and Services Administration). These disheartening statistics have started a discussion on why the gap between the number of organ donors and seekers has continued to widen and how a solution can be reached.
Currently in the US, organ donations are a result of donors specifically requesting to give their organ. Donors do not receive money for their donation, but rather contribute simply as an act of goodwill. Considering the system set in place, many suggestions have surfaced regarding possible changes that may result in an increase of donors. One perspective examines the role of choice in organ donation. If the system involved mandated choice, everyone would be required to explicitly make a decision about whether or not to donate, which may compel more people to consider giving an organ once they die. However, fears have been raised that if people opted to donate their organs, doctors may not put in their optimal effort to save those people’s lives in order to take advantage of their organ donation consent (University of Minnesota). Even when mandated choice was established in Texas in the 1990s, 80% of people chose not to be a donor (University of Minnesota). Another alternative is presumed consent, by which everyone is considered a donor unless otherwise specified. The main opposition with this idea is that it may be difficult for people with educational and other barriers to find a way to refuse donating if they choose to (University of Minnesota). A final proposition is to reward those who donate. Forms of compensation could include funeral coverage for deceased donors, commendations in the donor’s honor, and other rewards (University of Minnesota). The likeness of this system to a market and its implications on the poor have led to its downfall. Many more suggestions have been made to promote organ donations, but with the current system, the one change that could make a difference is to educate the public. Armed with more knowledge about how to donate, it may become possible to save more lives through organ donation.
Bibliography
Health Resources and Services Administration. “Organ Donation Statistics.” HRSA, 28 Sept. 2020, www.organdonor.gov/statistics-stories/statistics.html.
“Organ Transplantation.” Make a Stand, 23 Feb. 2020, www.make-a-stand.com/organ-transplantation-issues-and-solutions/.
University of Minnesota: Center for Bioethics. Ethics of Organ Transplantation. 1 Feb. 2004, conservancy.umn.edu/handle/11299/947.

Written by Christine Wan | Edited by Zainab Bhatti and Nicole Xu
What is HIPAA?
HIPAA is an acronym that stands for the 2003 Health Insurance Portability and Accountability Act. It is a United States law, developed by the Department of Health and Human Services, that provides privacy standards to protect patients’ medical records and other information that health plans, doctors, hospitals and other health care providers are allowed to access. These privacy standards provide patients with access to their medical records and allow patients greater control over the utilization and disclosure of their personal health information. HIPAA standards represent a uniform, federal set of privacy protections for patients nationwide and do not affect state laws that delineate additional protections (Shiel Jr.).
What are all the privacy standards covered under HIPAA?
The first provision is the privacy rule: this rule protects patients’ right to maintain the privacy of their health information, whether it be oral, written, or electronic health information. As an example, health providers must request a patient’s written authorization before sharing any health information with third party entities (Sobers). The main objective of this rule is to maintain a balance that permits the utilization of health information while protecting the patients’ privacy (Centers for Disease Control and Prevention).
The second provision is the security rule: this rule delineates rules for organizations to follow as a means to safeguard patients’ information. This rule details the technical, administrative safeguards required to protect electronic data only. As an example, there is authentication required to access healthcare providers’ networks and data systems (Sobers). This rule is put in place in order to ensure the confidentiality, integrity, and availability of all electronically-protected health information, detect and safeguard against anticipated threats to the security of the information, protect against anticipated impermissible utilization or disclosures, and certify compliance by the healthcare workforce (Centers for Disease Control and Prevention).
The third provision is the breach notification rule: this rule indicates that in the case of a data leak or security breach, patients must be notified within sixty days. If over five-hundred records are leaked or breached, healthcare providers are required to notify the Department of Health and Human Services (HHS). The HHS will then post the incident publicly on its website (Sobers).
The fourth provision is the enforcement rule: this rule illustrates the consequences of non-compliance to these privacy standards. In the case of a security breach, the healthcare provider in question will be fined (Sobers). Generally, HIPAA violations may result in civil monetary or criminal penalties (Centers for Disease Control and Prevention).
The fifth provision is the administrative simplification rule: this rule conveys that medical providers and health plans should standardize their health care transactions (Sobers).
Which entities are covered under HIPAA?
The following individuals and organizations are subject to the Privacy Rule and considered to be covered entities:
- Healthcare providers
- Health plans
- Exception: A group health plan with fewer than 50 participants that is administered solely by the employer that established and maintains that the plan is not a covered entity (Centers for Disease Control and Prevention).
- Healthcare clearinghouses: entities that process nonstandard information they receive from another entity into a standard
- Business associates: a person or organization using or disclosing health information to perform or provide functions, activities, or services for a covered entity
It is also important to note there are several permitted uses and disclosures of patient health information. For instance, covered entities are permitted to disclose health information without a patients’ authorization for health oversight activities, judicial and administrative proceedings, law enforcement, identification of deceased persons, victims of abuse, and the prevention of a serious threat to health and safety (Centers for Disease Control and Prevention).
Overall, though there are some risks, exceptions, and required disclosures inherent to protecting patients’ health information, there are several standards under HIPAA that aim to protect patient confidentiality as much as possible.
Bibliography
Centers for Disease Control and Prevention. “Health Insurance Portability and Accountability Act of 1996 (HIPAA).” Centers for Disease Control and Prevention, 14 Sept. 2018, www.cdc.gov/phlp/publications/topic/hipaa.html.
Sobers, Rob. “What Is HIPAA and Why Should I Care?” Inside Out Security, 30 Mar. 2020, www.varonis.com/blog/what-is-hipaa-and-why-should-you-care/.
William C. Shiel Jr. “Definition of HIPAA.” MedicineNet, 21 Dec. 2018, www.medicinenet.com/script/main/art.asp?articlekey=31785.

Written by Arathi Vinod | Edited by Sameer Rajesh and Nicole Xu
Exercise is considered the panacea for most of the biggest modern-day health conditions. By reducing body fat and weight, exercise plays a key role in preventing obesity, and in doing so, it also wards off serious heart conditions. The decrease in body fat allows the heart to put in less work to pump blood throughout the body, resulting in lower blood pressure and lower risk for cardiovascular disease. Exercise also encourages a wider range of motion, helping remedy muscle pain and joint pain. Above all, exercise has been observed to improve self-image and create a more positive outlook in individuals. In addition to these widely known advantages, exercise also has several understated benefits, providing all the more reason to adopt exercise as a daily practice.
Exercise and Learning
When considering the effects of exercise on muscles, the brain is likely not the first muscle that comes to mind. Nevertheless, exercise plays a significant role in molding neural circuits of the brain. Lifting weights or sprinting those final few yards access the same areas of the brain that learning does. For instance, both learning and exercise build upon concentration, long-term endurance, consequence evaluation, and motivation centers in the brain (Barile). Because of neural plasticity, the ever-changing nature of the brain, areas that are accessed more often tend to develop more. Therefore, by building on neural networks involved with focus, endurance, and motivation, exercise indirectly makes these pathways more accessible for learning as well.
Exercise also has more direct effects on learning. For example, through exercise, the body releases growth factors. These chemicals are responsible for producing new blood vessels to carry nutrients to the brain, as well as for sustaining the growth of brain cells (Godman). Brain studies align with these findings; the prefrontal cortex and medial temporal cortex, brain areas involved with memory, are more developed in individuals who exercise than in those who do not (Godman). Thus, not only does exercise improve the body, but it also has profound effects on the mind.
Exercise and Smoking
The connection between exercise and smoking is also often overlooked. Many of the symptoms associated with smoking withdrawal can be relieved by exercising. For instance, smokers often experience depression and lack of sleep when withdrawing from nicotine. Through the release of hormones such as dopamine and serotonin, exercise can counteract these withdrawal symptoms (Sandoiu).
Furthermore, research has shown that exercise increases the likelihood of quitting smoking. A study conducted by Dr. Alexis Bailey of St George’s University of London demonstrated that mice dependent on nicotine showed less dependency following exercise. Researchers divided up mice into three groups of varying exercise intensities (indicated by different amounts of time spent running on a wheel) and fed all mice in the study nicotine for two weeks. Upon observing withdrawal symptoms following the two weeks of study, the researchers found that mice who spent 2 hours or 24 hours per day running on the wheel showed less of the expected adverse effects than those that did not run on the wheel at all (Sandoiu). In fact, the brains of mice that exercised showed increased activity in alpha7 nicotinic acetylcholine receptors (special nicotine receptors) in the hippocampus, explaining why these mice did not experience such severe withdrawal symptoms.
Exercise and Cancer
Though cancers come in a variety of different forms, exercise has been shown to reduce the risk for many of these distinct cancers through indirect means. For instance, high body weight is often an indicator of high cancer risk. Visceral fat in low-oxygen conditions can result in inflammation, the body’s response to disease (Underferth). Inflammation increases cell reproduction, thereby increasing the chance of cell division going awry and becoming cancerous. Therefore, by decreasing body fat, exercise reduces the risk of cancers correlated with obesity, including breast cancer, uterine cancer, and pancreatic cancer (Underferth).
Hormone regulation is also integral in lowering the risk of cancer. Obesity and inflammation leads the body to make incorrect judgments about hormone needs, often secreting more than is needed. This then leads to further hormone imbalance; higher insulin levels trigger higher estrogen levels, and the amount of estrogen is further increased by secretion from fat cells. This rise in estrogen has been linked to conditions such as ovarian cancer and endometrial cancer (Underferth). Thus, physical activity plays a large part in preventing these cancers by not only decreasing the amount of fat cells, but also by regulating hormone levels and maintaining homeostatic conditions within the body.
Ultimately, though it has been widely accepted that exercise has a plethora of health benefits, research is still being conducted on the wide range of indirect effects it could have on more subtle health concerns. By altering the brain, regulating hormones, and decreasing body weight, exercise extends beyond simply physical benefits and shows potential for curing numerous other unforeseen health conditions.
Bibliography
Barile, Nancy. “Exercise and the Brain: How Fitness Impacts Learning.” Western Governors University, 16 Jan. 2018, www.wgu.edu/heyteach/article/exercise-and-brain-how-fitness-impacts-learning1801.html.
“Benefits of Exercise.” Medline Plus, 9 Oct. 2020, medlineplus.gov/benefitsofexercise.html.
Godman, Heidi. “Regular Exercise Changes the Brain to Improve Memory, Thinking Skills.” Harvard Health Publishing: Harvard Medical School, 26 June 2020, www.health.harvard.edu/blog/regular-exercise-changes-brain-improve-memory-thinking-skills-201404097110.
Sandoiu, Ana. “How Exercise Can Help You to Quit Smoking.” Medical News Today, 1 Jan. 2018, www.medicalnewstoday.com/articles/320484.
Underferth, Danielle. “How Does Obesity Cause Cancer?” MD Anderson Cancer Center, 8 May 2020, www.mdanderson.org/publications/focused-on-health/how-does-obesity-cause-cancer.h27Z1591413.html.

Written by Zeynep Demirag | Edited by Zainab Bhatti and Nicole Xu
Stigma is a set of negative beliefs and prejudices about a group of people. Many people face stigma because of their race, religion, sexuality, gender, and economic situation. People with mental illness often experience discrimination, and this can make them feel ashamed, hopeless, distressed, and reluctant to get help. This may also make those with mental illness reserved in accepting help and make them feel like they are to blame for their illness. Research on stigma shows that although people understand and acknowledge the medical and genetic nature of mental disorders, they still maintain a negative view of those with mental disorders.1 The American Psychiatric Association identifies three different types of stigma: public stigma, self stigma, and institutional stigma. Public stigma is when one faces discrimination or negative attitudes by other people. Self stigma is the internalized shame that people with mental illness have about their own condition while institutional stigma is more systemic, involving government and private organization policies that intentionally or unintentionally limit opportunities for people with mental disorders. Examples include lower funding for mental illness research or fewer mental health services relative to other health care services.2
Oftentimes other people’s judgment about mental illnesses comes from a lack of knowledge about peoples’ situations. According to the American Psychiatric Association, when we know someone with mental illness, mental disorder becomes less scary and more real or relatable.2 A 2016 review of research showed that an effort to reduce mental health stigma is evidently making it better internally and on a populational level. The strongest evidence was for anti-stigma efforts involving those with lived mental health experiences and efforts with a long-term commitment.3
Here are some suggestions from The National Alliance on Mental Illness (NAMI) about what you can do as an individual to unlearn mental illness :4
- Talk openly about mental health, such as sharing on social media in a constructive way. A 2020 survey suggests that 90% of adolescents and young adults who experience depression are researching mental disorders online and accessing other people’s podcasts, blogs, and videos.3
- Educate yourself and others. Respond to misperceptions or negative comments by sharing facts and experiences.
- Be conscious of language. Remind people that language is powerful and let others know when they are using stigmatizing language or presenting mental illness in a stigmatizing way. Remember, unlearning stigma is more important than learning what to do about it
- Encourage equality between physical and mental illness. Draw comparisons to how others would treat someone with visible illnesses such as cancer or heart disease
- Show compassion for those with mental illness – they are not avoiding you, rather they might be struggling to cope with a mental illness.
- Normalize mental health treatment – there are no anti-cardiology movements or movements trying to ban cancer treatment, but there is a virulent anti-psychiatry movement that disclaims mental illness
- Choose empowerment over shame – your mind is more important than what others think about you
1 Vigo, Daniel. “The health crisis of mental health stigma.” Lancet 3 (2016): 171-178
2Borenstein, Jeffrey. “Stigma, Prejudice and Discrimination Against People with Mental Illness.” American Psychiatric Association, Aug. 2020, www.psychiatry.org/patients-families/stigma-and-discrimination.
3Center for Workplace Mental Health. Working Well Toolkit. 2016.4
4 “Mental Illness.” National Institute of Mental Health, U.S. Department of Health and Human Services, Nov. 2020, www.nimh.nih.gov/health/statistics/mental-illness.shtml.

Written by Athira Vinod | Edited by Sameer Rajesh and Nicole Xu
The US healthcare system has been under scrutiny for years in regards to various factors, such as cost, accessibility, and overall quality. The merits and drawbacks of the healthcare system in the US can be studied through comparison with the systems in other countries. Healthcare in the United States can be broken down into four major components: private insurance, Medicare, Medicaid, and the VA. Most Americans get private insurance from their employers, which can cover preventive care, prescription drugs, and treatment for illnesses1. A smaller percentage of people have Medicare and Medicaid. Medicare is a service opted for by many older citizens, and consists of several subdivisions involving hospitalization, outpatient services, prescription drug plans, or other benefits1. Unlike Medicare, which is a federal government-run program, Medicaid is administered by the state. Medicaid is generally reserved for those with lower socioeconomic status, and for the most part, those who also have children1. Because of the requirement of having children and the very low poverty cutoff, not all people who are financially struggling are qualified for Medicaid. Finally, the VA includes the government-run Veterans Health Administration as well as the private program Tricare, both of which benefit veterans1.
In contrast to the United States, many other countries do not emphasize the private over the public component of healthcare. In Canada, as much as 70% of healthcare is paid for by the government1. Apart from care involving drugs, dentistry, and optometry, the Canadian government is largely responsible for covering healthcare, making this a Single Payer system1. Many other countries, especially in Europe, have universal healthcare instead. Australia is one such country; unlike the US healthcare system of the same name, Australian Medicare covers not only the elderly, but also residents, visiting students, and those seeking asylum1. Universal healthcare guarantees some fundamental coverage for everyone, beyond which citizens would be able to opt for additional coverage. This contrasts starkly with America, where a considerable portion of the population is uninsured1. One potential drawback of the universal healthcare system is that since more people are insured, it may take longer for one to meet with his/her physician2.
The merits of the US healthcare system in relation to other parts of the world can be gauged by weighing its costs and benefits. The United States spends significantly more on healthcare than other countries. Compared to the $5,500 average per capita healthcare spending of other wealthy countries, America spends over $11,000. Specifically, it has been shown that the US spends considerably more than other countries on the administrative aspects of healthcare, but spends much less than other countries on long-term care3. The high costs of healthcare in the US can be explained by several factors. The advancement of technology in the medical field is one factor that can account for the rise in costs3. In addition, the monopoly of hospitals and the subsequent lack of competition may also have a large part in driving up the price of healthcare3. The strikingly high healthcare expenditures can be measured against health outcomes in order to evaluate the quality of the healthcare system in the US. Although the US shows better outcomes in some areas, like heart rate mortality, it shows poor outcomes in others, including infant mortality, unmanaged diabetes, and safety during childbirth3. This widely varying range of health outcomes suggests that despite the high costs paid for healthcare, the system in the US is not as effective as it could be in ensuring citizens’ wellbeing. Looking to the systems established around the world may provide insight on future changes in healthcare.
1Healthcare Triage. “Healthcare Systems In The U.S. And Other Countries Explained: Healthcare Triage.” Web. 09 Nov. 2020.
2McLachlan, Natasha. “U.S. Health Care vs Health Care Systems in Other Countries US Insurance Agents.” 06 Nov. 2020. Web. 09 Nov. 2020.
3Peter G. Peterson Foundation. “How Does the U.S. Healthcare System Compare to Other Countries?” 14 July 2020. Web. 09 Nov. 2020.

Written by Christine Wan | Edited by Zainab Bhatti and Nicole Xu
Gender disparities within the medical and academic worlds are becoming increasingly apparent. Several studies have even identified significant gender discrepancies in grant funding, leadership positions, and publications’ impacts in surgical subspecialties, such as vascular surgery. For instance, one such study focuses on the disparities within the realm of academic vascular surgery. This study ultimately concludes that although there appears to be greater representation of women in the realm of academic vascular surgery now relative to decades ago, discrepancies still exist. Women not only receive fewer grants and industry payments1 compared to men, women still hold fewer leadership positions, such as chief of surgery, and are not published or cited nearly as often as their male colleagues. In fact, only 11% of vascular surgeons are women, and these women have 35% fewer publications compared to their male counterparts. Research papers written by women are even cited less than half as often as research conducted by male surgeons (Carnevale et al).
Moreover, people are increasingly shedding light not only on just sexism, but also on coded sexism2 within the medical and academic communities. An article published, and later retracted, by the Journal of Vascular Surgery provides an example of blatant coded sexism in the medical community. The article, written and reviewed by mainly male authors, centers on “unprofessional” and “provocative” social media content, most of which were posted on female physicians’ personal accounts (Hardouin). The editorial board ultimately stated, after further review, that the article presents issues, including gender bias and infringement of privacy, which prompted the journal to retract this article (Shapiro). Nevertheless, such occurrences are gaining greater traction due to the increasing spread of such information through social media as well as the hashtag: #MedBikini.
Through this hashtag and other forms of backlash against the article, the authors addressed the blatant issues of patient privacy and uncollegial behavior. However, according to Shapiro, the focus on female surgeons wearing bikinis, especially tracked by male students and colleagues under fake social media accounts, is aligned with the “creep” factor. With the rise of another hashtag, #ILookLikeASurgeon, it has increasingly been emphasized that those who are bikini-clad, of all-shapes-and-size, and of all genders regardless of identity can be surgeons. The #MedBikini trend has aimed to humanize, not deprofessionalize, women in a traditionally male profession (Shapiro).
As such, the utilization of social media and other forms of media has largely aided in shedding light on issues like sheer sexism within the medical community and has even worked to push against these issues.
1. Industry Payments: payments or investments sponsored by healthcare industries (Carnevale et al.)
2. Coded Sexism: sexism that is relatively less blatant and apparent; can be rooted in definitions of professionalism or, rather, unprofessionalism (Shapiro). For instance, coded sexism is involved regarding claims that young women physicians’ private social media account posts, such as their bikini posts, were “unprofessional.”
Bibliography
Carnevale, Matthew et al. “Gender disparities in academic vascular surgeons.” Journal of vascular surgery vol. 72,4 (2020): 1445-1450. doi:10.1016/j.jvs.2019.12.042
Hardouin, Scott et al. “RETRACTED: Prevalence of unprofessional social media content among young vascular surgeons.” Journal of vascular surgery vol. 72,2 (2020): 667-671. doi:10.1016/j.jvs.2019.10.069
Shapiro, Nina. “Viral #MedBikini Response To Controversial Manuscript Leads Editor To Retract Article.” Forbes, Forbes Magazine, 25 July 2020, www.forbes.com/sites/ninashapiro/2020/07/25/viral-medbikini-response-to-controversial-manuscript-leads-editor-to-retract-article/?sh=62996cc11f47.
Written by Arathi Vinod | Edited by Sameer Rajesh and Nicole Xu
Technology has become so ingrained in the practice of healthcare that we often fail to give it the admiration it deserves. From small digital thermometers used in households to virtual reality programs now being implemented by surgeons in training, technological advancements in medicine are integral to improving both the efficiency of doctors and the well-being of patients. Two aspects of technology that have impacted healthcare in major ways are new medical equipment and medical information systems.
Equipment Technology
Medicine has become a center of rapid technological development. One particular realm of interest is imaging. Magnetic Resonance Imaging, or MRI, uses an extremely strong magnet and radio waves to image organs in a patient. The magnetic field produced by the magnet helps align atoms in the vicinity of the organ, and when a radio wave is directed at the atoms, the protons in the atoms activate and shift position. When the radio waves are turned off, the protons return to their previous positions and realign with the magnetic field, releasing energy. The amount of energy released by different protons gives information about what kinds of tissues are present in the area being imaged (“Magnetic Resonance Imaging (MRI)”). Another common imaging tool is mammography. Using plates to flatten the area of study, mammography utilizes x-rays to detect irregularities in the breast. Differences in tissue density appear as different colors on the resulting mammogram, and potential tumors appear as white areas (“Mammography”). Imaging technologies like MRI and mammograms are crucial tools for doctors to use in assessing regions in the body that are otherwise inconvenient to reach or difficult to study without using invasive measures.
Artificial organs represent another significant technological innovation. Artificial limbs are engineered to simulate the ranges of motion of their real counterparts, offering patients who have lost limbs due to accidents or genetic diseases a way to return to their normal lives. Techniques like 3-D printing have greatly facilitated this process, allowing for more precision in the creation of prosthetic limbs. However, prosthetics are not the only successes of bioengineering; other artificial organs are essential to patients in critical conditions. Dialysis machines work as artificial kidneys to filter the blood, serving as a source of comfort for patients suffering from diabetes, lupus, and a multitude of other kidney disorders . Artificial hearts are another frontier to further explore within bioengineering. Though few have been implemented as permanent solutions for replacement hearts , the prospect of further developing the artificial heart is exciting and offers a potential solution for individuals who are unable to safely receive transplants (“Innovations in Artificial Organs”).
Information Technology
Though technology in medicine calls to mind large machines and futuristic contraptions, many of the remarkable innovative methods widely used today are more subtle. Information technology has revolutionized the practice of healthcare by increasing access for patients and facilitating medical practices for doctors. For instance, the concept of telehealth has been groundbreaking in healthcare. Through telemedicine, physicians are able to communicate with their patients and track their progress without having to actually meet with them in person (“Medical Technology”). This is particularly vital for those who do not have access to a local hospital or clinic and ultimately helps alleviate health disparities. Telehealth is more important today than it has ever been. Through methods like contact tracing over the phone, health practitioners are able to utilize telehealth to track potential COVID-19 carriers and give medical advice to affected individuals without having to engage in in-person contact.
Information technology has also proven immensely beneficial to the patient tracking process. Electronic health records, or EHRs, are a way of storing patient records on a computer rather than on physical paper files (“5 Ways Technology is Improving Health”). Following generations of traditional record-keeping, this new method has emerged as a cost-effective way for hospitals to keep track of accurate patient information. In addition to their financial benefits, EHRs also facilitate patient tracking for physicians, allowing them to quickly access a patient’s medical histories and easily transfer important patient information to other medical specialties that the patient requires.
Medical technology is actively in use today for the purpose of medical research. Through techniques like genomic sequencing and the meticulous, long-term record-tracking enabled by technology, researchers are now able to make advancements in medicine that were previously thought impossible. Thanks to the power of impressive technological innovations, the field of healthcare is more accessible, smart, and efficient than ever before.
Bibliography
“5 Ways Technology Is Improving Health: UIC Health Informatics.” UIC Online Health Informatics. 13 July 2020. Web. 03 Nov. 2020.
“Innovations in Artificial Organs.” The Alliance of Advanced BioMedical Engineering. Web. 03 Nov. 2020.
“Magnetic Resonance Imaging (MRI).” National Institute of Biomedical Imaging and Bioengineering. U.S. Department of Health and Human Services. Web. 03 Nov. 2020.
“Mammography.” National Institute of Biomedical Imaging and Bioengineering. U.S. Department of Health and Human Services. Web. 03 Nov. 2020.
“Medical Technology.” Healthcare Business & Tech. 23 Dec. 2011. Web. 03 Nov. 2020.

Written by Zeynep Demirag | Edited by Zainab Bhatti and Nicole Xu
Health is the state of physical, social, and mental well being–not just the absence of disease and infirmity. It is also something we want to achieve not just individually but as a community. Health determinants include one’s age, gender, genetic makeup, and health behaviors. Health behavior examples include smoking, drinking, diet, and physical activity. Health is also largely influenced by social determinants, most commonly defined as the conditions in which people are born, live, learn, work, play, worship, and age that affect health outcomes.1
Social determinants of health are shaped by the distribution of money and power resources on international, national, and local levels. Consequently, social determinants can lead to health inequalities.2 According to the framework developed by the World Health Organization (WHO), social determinants of health are defined within two broad groups: structural determinants and intermediary determinants. Structural determinants are the socioeconomic and political contexts that people live in. These contexts include governance, economics, social and public policies, as well as social and cultural values placed on health issues. These factors can lead to the unequal distribution of material and monetary resources which can shape a person’s socioeconomic position. Socioeconomic position is characterized by a multitude of factors including: education, occupation, income, gender, race or ethnicity, and social class. The structural determinant of health operates through a set of intermediary determinants that impact a person’s exposure, vulnerability and health outcomes. These include material circumstances, such as the quality of housing, financial means to buying healthy food, adequate clothing, and other requirements for healthy living. Intermediary determinants also include psychosocial factors such as stressful living circumstances, relationships, and amount of social support.2
In addition to what is discussed above, health systems determine the type, quality, and accessibility of health care. Bridging the structural and intermediary determinants are social cohesion and social capital. The links between all these determinants are not always linear. They can be complex and interdependent–interacting in many different ways to influence health. For example, poor income can limit opportunities for achieving good health, and conversely, poor health can limit opportunities for people to participate in the workforce. Moreover, these determinants can act differently across the course of a person’s life.2 Therefore, when thinking of a health issue, it is important to not only consider who an individual is and what they do, but to also consider the conditions in which they are born, grown, live, work, and age. If we understand and act on these factors we can build a healthier world for everyone.3
Bibiliography
1Healthypeople.gov. 2020. Social Determinants Of Health | Healthy People 2020. [online] Available at: <https://www.healthypeople.gov/2020/topics-objectives/topic/social-determinants-of-health> [Accessed 4 November 2020].
2Who.int. 2020. Social Determinants Of Health. [online] Available at: <https://www.who.int/teams/social-determinants-of-health> [Accessed 4 November 2020].
3Who.int. 2020. Constitution. [online] Available at: <https://www.who.int/about/who-we-are/constitution> [Accessed 4 November 2020].

Written by Athira Vinod | Edited by Sameer Rajesh and Nicole Xu
Obesity is a health issue that has been on the rise in recent years. Generally defined by a body mass index of 30.0 or higher, obesity is an indication of higher than healthy levels of body fat (Mayo Clinic). Considering the prevalence of this condition in the United States, an extensive look into the causes of obesity is much needed.
Potential contributors to obesity can look different for everyone. One of the most commonly cited factors of the condition is a poorly balanced diet. Consuming large portions of foods high in fats or carbohydrates can lead to weight gain (Nammi et al.). Although committing to a healthier diet may appear to be a simple solution to these concerns, it is important to consider the various components that play a part in going through with such plans. For instance, a restrictive diet plan may further contribute to an increased urge to eat more frequently (Nammi et al.). Alternatively, one’s living conditions may not permit the luxury of finding quality fruits and vegetables, which would force them to turn to a less than ideal diet (Pan et al.). An unbalanced diet becomes a more potent predictor of obesity when combined with a sedentary lifestyle. The lack of exercise prevents the burning of calories taken in through meals, leading to a rise in weight gain. One’s life situation can have an immense effect on this factor; staying active becomes a much less attainable goal if one’s schedule does not allow for it, or if one’s surroundings do not hold safe spaces for exercise (Pan et al.).
Although most conversations about obesity center around diet and exercise, there are several other facets to the condition. The genetic component of obesity is often overlooked, despite being a significant contributor. Implementing changes in food consumption or adopting a more active lifestyle may not produce as notable a change in some compared to others. One main reason for this may be that the individual’s fat distribution or ability to burn calories matches that of their parents (Hampton). Genetic factors such as these can have a sizable impact on where one’s BMI stands. It is also worth noting that similarities in weight among family members can be attributed to lifestyle and eating behaviors that are shared within the family (Nammi et al.). Apart from these environmental influences, however, genetic predispositions to obesity can reveal themselves in the form of diseases that can directly or indirectly increase the likelihood of obesity. The need for medications or the inability to walk, for example, can lead to an increase in weight over time (Mayo Clinic).
Like all conditions and diseases, obesity has many overlapping causes that can all contribute in some form to weight gain. In order to lower the rate of obesity, it is essential that these underlying factors be taken into consideration when planning healthy lifestyle changes. Although a variety of elements can influence the development of obesity, managing the controllable factors can be a major stepping stone to a longer and healthier life.
Bibliography
Hampton, Tracy. “Role of Genes in Obesity and Fat Distribution.” JAMA, JAMA Network, 7 Apr. 2015, jamanetwork.com/journals/jama/article-abstract/2214075.
Mayo Clinic. “Obesity.” Mayo Clinic, Mayo Foundation for Medical Education and Research, 15 Feb. 2020, www.mayoclinic.org/diseases-conditions/obesity/symptoms-causes/syc-20375742.
Nammi, Srinivas, et al. “Obesity: An Overview on Its Current Perspectives and Treatment Options.” Nutrition Journal, BioMed Central, 14 Apr. 2004, nutritionj.biomedcentral.com/articles/10.1186/1475-2891-3-3.
Pan, Liping, et al. “Food Insecurity Is Associated with Obesity among US Adults in 12 States.” Journal of the Academy of Nutrition and Dietetics, U.S. National Library of Medicine, Sept. 2012, www.ncbi.nlm.nih.gov/pmc/articles/PMC4584410/.

Written by Christine Wan | Edited by Zainab Bhatti and Nicole Xu
Telemedicine involves the utilization of electronic information as well as telecommunication technology so that patients can obtain the healthcare they need while maintaining social distancing guidelines (Centers for Disease Control and Prevention). In fact, several healthcare providers and programs have adopted telemedicine platforms and associated technology in order to decrease patients’ interaction with healthcare facilities, other patients, and healthcare staff. This ultimately serves as a means to reduce patients’ and all related personnel’s risk for COVID-19 (Centers for Disease Control and Prevention).
With regards to telehealth modalities, there are three prominent types, all of which allow HealthCare Partners (HCP) or healthcare professionals and patients to connect through technology. One of the three modalities is called synchronous: this method involves real-time telephone or live audio-video interaction and usually occurs through a smartphone, tablet, or computer. In certain cases, peripheral medical equipment (digital stethoscopes, otoscopes, ultrasounds) is utilized by HCP, like nurses, who physically interact with the patient as the consulting medical provider calls in to conduct a remote evaluation. As such, contact is decreased as the patient only interacts with the nurse, rather than both the nurse and the consulting medical provider. Another modality is called asynchronous: this modality involves “store and forward” technology; messages, images, or data that are previously collected are interpreted or responded to at a later date. Moreover, patient portals can facilitate this method of communication between providers and patients through a secure messaging system. The third modality is called remote patient monitoring: this modality involves direct transmission of a patient’s clinical measurements from a distance to their healthcare provider and does not necessarily occur in real-time (Centers for Disease Control and Prevention).
In particular, telehealth services can be used to screen patients who may have symptoms of COVID-19, provide low-risk urgent care for non-COVID-19 conditions, and increase access to primary care providers and specialists. This would include mental and behavioral health specialists as well as specialists for chronic health conditions and medication management. Specific examples of the utilization of telehealth services are weight management and nutrition counseling. Other types of therapy offered remotely have included physical therapy and occupational therapy through hybrid modality approaches. Telemedicine has also provided greater access to those who live in very rural settings, older adults, and those with limited mobility. Other uses of telemedicine include general health care, like wellness visits and advice about certain non-emergency illnesses, medication prescription, and mental health counseling (Centers for Disease Control and Prevention).
In addition to greater accessibility for certain patient groups, there are other benefits to utilizing telemedicine. For example, telemedicine allows patients to access their physicians with greater ease. With telemedicine, patients are able to speak with their physicians live over the phone or video chat and physicians are able to remotely monitor their patients. Other advantages include saving both time and transportation costs to the healthcare facilities as well as the reduced wait time for services and reduced number of visits to clinics. Additionally, telehealth services have facilitated public health mitigation strategies amidst the COVID pandemic by increasing social distancing and reducing interaction and contact between providers and patients. Telemedicine has also been able to decrease strain on healthcare systems by directly reducing patient demand on facilities. Moreover, telemedicine is able to provide adequate continuity of care, preventing negative consequences associated with delayed preventive, chronic, or routine care. The utilization of remote access to healthcare has also aided with the preservation of patient-provider relationships when in-person visits are unfeasible (Centers for Disease Control and Prevention).
Many healthcare and insurance programs have adapted to the above-mentioned telemedicine modalities as well as to the rise of telemedicine. For instance, the Health Insurance Portability and Accountability Act (HIPAA) has become increasingly flexible throughout the duration of COVID-19. In accordance with the HHS Office for Civil Rights (OCR) guidelines that empower health care providers to serve patients through telehealth, HIPAA-covered healthcare providers have increasingly provided telehealth services to patients. These providers have utilized remote communication technologies, including FaceTime, Facebook Messenger, Google Hangouts, Zoom, and Skype, to offer telehealth services. Moreover, the Centers for Medicare & Medicaid Services (CMS) has issued temporary measures to allow people to enroll in Medicare, Medicaid, and the Children’s Health Insurance Program (CHIP) with greater ease, providing these people with greater access to medical care. CMS has also expanded the list of covered telehealth services to include more services, like home visits and therapy services (U.S. Department of Health & Human Services).
Through COVID, healthcare has transformed through the increasing use of telemedicine, which has, in itself, experienced transformations. In particular, there have been several innovative uses of telemedicine as well as advances in telehealth platforms that have ultimately allowed HCP to better aid patients through remote patient monitoring technology and other facets. These other sources of innovation include new mobile health apps and wearable monitoring devices. These monitoring devices aid in tracking patients’ vitals, providing alerts about necessary care, and aiding patients in accessing their respective physicians (Verma). As such, healthcare and technology have risen to meet the evolving needs of healthcare in light of changing conditions.
Bibliography
Centers for Disease Control and Prevention. “COVID-19: Telemedicine – What Does It Mean and Why Should You Care?” Centers for Disease Control and Prevention, Centers for Disease Control and Prevention, 15 Sept. 2020, www.cdc.gov/coronavirus/2019-ncov/global-covid-19/telemedicine.html.
Centers for Disease Control and Prevention. “Using Telehealth to Expand Access to Essential Health Services during the COVID-19 Pandemic.” Centers for Disease Control and Prevention, Centers for Disease Control and Prevention, 10 June 2020, www.cdc.gov/coronavirus/2019-ncov/hcp/telehealth.html.
U.S. Department of Health & Human Services. “Telehealth: Delivering Care Safely During COVID-19.” HHS.gov, U.S. Department of Health and Human Services, 15 July 2020, www.hhs.gov/coronavirus/telehealth/index.html.
Verma, Seema. “Early Impact Of CMS Expansion Of Medicare Telehealth During COVID-19.” Health Affairs, Project HOPE, 15 July 2020, www.healthaffairs.org/do/10.1377/hblog20200715.454789/full/.

Written by Arathi Vinod | Edited by Sameer Rajesh and Nicole Xu
For many, the word malnutrition quickly brings to mind the image of undernourished children in developing countries, experiencing hunger as a result of a severe lack in resources. However, contrary to popular belief, malnutrition encompasses a wide range of conditions resulting from a complex web of circumstances, and every country in the world is vulnerable to it. Regardless of the various forms and causes of malnutrition, though, one thing is certain: nutrition equity is quickly becoming a significant health concern across the world.
One critical condition that falls under malnutrition is undernutrition. Classified based on weight-to-height ratio, weight-to-age ratio, or height-to-age ratio, undernutrition is evident through wasting, underweight, and stunting respectively (“Malnutrition”). As expected, undernutrition is the result of a persistent lack of food, either due to an environment scarce in nutrients or due to diseases that cause a decrease in food intake. However, even if nutritional needs are mostly being met, malnutrition can occur if particular vitamins and minerals are not consumed. Known as micronutrient-related malnutrition, this type of malnutrition commonly targets individuals lacking essential nutrients such as iron, iodine, and Vitamin A (“Malnutrition”). Deficiencies in such vitamins or minerals can have devastating impacts on the individual’s health. For instance, thyroid hormones depend on a surplus of iodine in the diet to help maintain metabolism, and if the body experiences iodine deficiency, the thyroid gland will not be able to produce enough hormones, leading to hypothyroidism (“Iodine Deficiency”). Finally, the third form of malnutrition is overweight and obesity. Like undernutrition, overweight and obesity are also tracked by weight-to-height ratios, through measurements of BMI, or body mass index. A BMI of 25 or more is considered overweight, and 30 or over is classified as obese (“Malnutrition”). These conditions are caused by the overconsumption of energy-rich foods, accompanied by a deficiency in other food types and a lack of physical movement. The buildup of visceral fat caused by overweight and obesity is the root of a multitude of serious health conditions, most notably heart disorders and type 2 diabetes.
In short, malnutrition can be summed up as a lack of food security, which is defined by the Food and Agricultural Organization of the United Nations as a state when individuals always have “‘physical and economic access’” to food that is “‘sufficient, safe and nutritious’” (Fanzo). All three forms of malnutrition can be broken down using the social determinants. There are officially five components to the Social Determinants of Health (SDOH): economic stability, education, health care access and quality, neighborhood and built environment, and social and community context (“Social Determinants of Health”). Contextualizing these determinants within the topic of nutrition equity, the potential origins of malnutrition can be deduced. Perhaps most apparently, environment and socioeconomic status can play a key role in an individual’s malnutrition, either because of a literal shortage of food in the area, or because of the large part wealth plays in access to nutritious food. However, there are also more subtle causes of food insecurity. For example, cultural values and societal norms might directly or indirectly enforce eating behaviors that are detrimental to the individual (“Towards Global Nutrition Equity”). Furthermore, there is a significant political facet to nutrition equity; the institutions and policies set in place by the government have a large say in the types of food that individuals have access to and grow up with, influencing the nutritional choices that they then pass on to the next generation.
Fortunately, many policies have been put forth in recent years to try to combat these deep-rooted causes of nutrition inequity. For instance, the United Nations began a program called Decade of Action on Nutrition in 2016, through which they hope to eliminate malnutrition by the year 2025 by taking all the actions necessary to guarantee food security for everyone (“Towards Global Nutrition Equity”). Other policies aim to relieve the effects of malnutrition. The Medical Nutrition Equity Act (MNEA) is a piece of legislation introduced in 2019 that hopes to allow insurance coverage for those with nutrition-deficiency related disorders, including digestive conditions like malabsorption and inherited conditions like phenylketonuria (“Medical Nutrition Equity Act”). Through such well-meaning endeavors, as well as a resolve to continue understanding and spreading awareness about the complexities of malnutrition, there is still hope for the world to achieve nutrition equity.
Bibliography
Fanzo, Jess. “A Piece of the Pie in Health Equity: Improving Food & Nutrition Security.” Johns Hopkins Alliance for a Healthier World, Johns Hopkins Alliance for a Healthier World, 14 July 2018, www.ahealthierworld.jhu.edu/ahw-updates/2018/7/13/a-piece-of-the-pie-in-health-equity-improving-food-nutrition-security.
“Iodine Deficiency.” Temple Health, 2020, www.templehealth.org/services/conditions/iodine-deficiency.
“Malnutrition.” World Health Organization, World Health Organization, 1 Apr. 2020, www.who.int/news-room/fact-sheets/detail/malnutrition.
“Medical Nutrition Equity Act – Action Needed!” APFED, 17 Mar. 2020, apfed.org/advocacy/medical-nutrition-equity-act/.
“Social Determinants of Health.” Office of Disease Prevention and Health Promotion, US Department of Health and Human Services, health.gov/healthypeople/objectives-and-data/social-determinants-health.
“Towards Global Nutrition Equity.” Global Nutrition Report, 2020, globalnutritionreport.org/reports/2020-global-nutrition-report/introduction-towards-global-nutrition-equity/.

Written by Zeynep Demirag | Edited by Zainab Bhatti and Nicole Xu
Can anyone explain health insurance in one sentence? Most likely not. Health insurance, just as most things health related, is nuanced and complex. This article will cover important keywords, the different types of health insurance, crucial features of payment, and essential benefits that every health insurance plan should provide. Health insurance, in its most basic form, helps protect you from paying the full cost of your health care. Five crucial terms to understand include1:
Network: Your health insurance has a group of providers that are in their network. Using physicians at hospitals in your insurance company network will keep your out of pocket cost lower; insurance companies will have lower/no benefits for out of network providers.
Premium: The amount you pay to your company each month to keep your membership active. A higher premium can lower out of pocket expenses and vice versa.
Deductible: The amount you pay every year before your health insurance pays for a portion of your services. For example, if you have a $2000 medical bill, and your plan has a $800 deductible, the first $500 will be your deductible and then your insurance company will pay their portion for the remaining $1500.
Co-pay: The fixed cost you pay before each visit. This amount does not go towards your deductible.
Co-insurance: The rate of the cost you would pay after the deductible. Going back to our example: if your co-insurance rate is10% then you would pay $150 from the $1500 remaining after deductible.
Out of pocket maximum: Maximum amount of money you pay for covered services.
Types of Health Insurance:
There are usually two types of health insurance: public and private insurance one purchases or gets it through their employer. Popular names for public insurance include CHIP, Medicare, Medicaid. Private health insurance also contains a variety of different plans2:
HMO (Health Maintenance Organizations): HMO members need to get a referral to go to a specialist from their primary care physician . HMO is the most restrictive plan to access a wide range of providers and will not cover out of network providers, however, they have the lowest premium.
PPO (Preferred Provider Organization): Unlike HMO, this plan gives you a greater range of doctors and more accessibility to out of network providers. PPO will pay for out of network providers but your premium will be higher than for HMO. PPO members do not need referrals from their primary care physician to see a specialist.
EPO (Exclusive Provider Organization): Think of this as something in between HMO and PPO, price-wise and accessibility-wise. You may see a specialist without a referral; however, depending on your plan, out of network will not be covered by the private insurance.
POS (Point of Service): Again, think of this as something in between HMO and PPO. You will need a referral for a specialist, but you may also see out of network providers depending on your plan.
*See more detailed comparison between these plans here*
Benefits that Every Plan Should Provide:
According to the US Department of Health and Human Services, you should be getting coverage and benefits for services listed below regardless of your plan3:
1- Ambulatory patient services
2-Emergency services
3-Hospitalization
4-Pregnancy, maternity, and newborn care
5-Mental Health and substance use disorder services
6-Prescription drugs
7-Rehabilitative and habilitative services and devices
8-Laboratory services
9-Preventive and wellness services
10-Pediatric services including oral and vision care (note that adult dental and visual services are not considered as essential health benefits)
Bibliography:
1. “Type of Plan and Provider Network.” HealthCare.gov, www.healthcare.gov/choose-a-plan/plan-types/.
2. “How to Understand Your Costs and Key Health Insurance Terms.” HealthCare.gov, www.healthcare.gov/blog/understand-health-insurance-definitions/.
3. “Find out What Marketplace Health Insurance Plans Cover.” www.healthcare.gov/coverage/what-marketplace-plans-cover/.

Written by Athira Vinod | Edited by Sameer Rajesh and Nicole Xu
When advocating for the overall wellbeing of the community, it is important to consider the opportunities available to each and every individual encompassed by that community. In the US today, however, people of certain identities are more vulnerable to health conditions because of the disparities that exist in healthcare. Health disparities can generally be defined as differences in access to quality healthcare across groups of people. Being a part of minority groups in relation to socio-economic status, sexual orientation, education, and race, among others can put one at risk of receiving a reduced level of medical care.
Although health disparities can emerge from a variety of differences in identity and lifestyle, racial and ethnic minorities in particular have suffered greatly in terms of health disparities. These groups have faced worse health consequences for decades as a result of differential treatment. The Heckler Report, created by US Health and Human Services Secretary Margaret M. Heckler, was a critical turning point in the conversation around racial and ethnic disparities (Riley). Released in 1985, the report initiated a dialogue about health disparities among racial minorities, addressing a longstanding problem for the first time. The Heckler Report brought alarming inconsistencies in medical care to attention. It claimed, for instance, that 45% of black deaths (age 70 or below) could have been avoided if better medical attention was offered (Riley). The report’s explicit listing of such statements instigated the conversation around health disparities in race that is still very alive today. When considering the severe decline in the health and life expectancy of racial minority groups, it is clear that discrimination and prejudice are at the root of this lack of access to healthcare. Biases, implicit and otherwise, have resulted in inadequate methods of testing, evaluation, and care among racial and ethnic minorities.
Efforts have since been made to bridge the gaps in differential medical care within the US. In 2013, the Institution of Medicine took on the initiative of reviewing renowned medical studies and articles for racial bias and subsequently explained their findings in a report as proof of health disparities (Riley). In addition, as a proactive attempt to erase the disparities in treatment of individuals from various backgrounds, organizations like the American Medical Association have also provided resources to guide physician treatment of all people, including tools to best help various populations, such as the disabled community (“Reducing Disparities in Health Care”). However, there are still several challenges that must be overcome to remove health disparities, one of the most significant being the cost of healthcare, which stands as an obstruction to those from lower socio-economic backgrounds seeking health insurance coverage (Woolf and Braveman, et al). Additionally, the persistent belief that differences in care are contrived has hindered the fight against health disparities. Continuing these efforts is essential in furthering the possibility of more equal grounds in healthcare.
Bibliography
“Reducing Disparities in Health Care.” American Medical Association, www.ama-assn.org/delivering-care/patient-support-advocacy/reducing-disparities- health-care.
Riley, Wayne J. “Health Disparities: Gaps in Access, Quality and Affordability of Medical Care.” Transactions of the American Clinical and Climatological Association, American Clinical and Climatological Association, 2012, www.ncbi.nlm.nih.gov/pmc/articles/PMC3540621/.
Steven H. Woolf and Paula Braveman, et al. “Where Health Disparities Begin: The Role Of Social And Economic Determinants-And Why Current Policies May Make Matters Worse.” Health Affairs, 1 Oct. 2011, www.healthaffairs.org/doi/full/10.1377/hlthaff.2011.0685.

Written by Christine Wan | Edited by Zainab Bhatti and Nicole Xu
Medicare and Medicaid are oftentimes confused and used synonymously. However, these two programs bear fundamental differences. Each measure is regulated by laws and policies unique to that particular program and is specifically designed for different populations.
The most evident difference between these two programs lies in the types of people who qualify for them as well as the purpose each measure serves. In regards to Medicare, this measure is an insurance program, in which medical bills are paid from trust funds that individuals with such coverage have paid into. Regardless of income level, all U.S. citizens over the age of 65 who have difficulty covering expenses related to medical care and treatment are aided by Medicare (Mitchell & Potter). This measure, however, also serves younger patients with specific illnesses, including end-stage renal disease (ESRD) and amyotrophic lateral sclerosis (ALS), also called Lou Gehrig’s Disease (Masterson). Patients pay a portion of costs through deductibles1 for hospital costs, while monthly premiums2 are required for non-hospital coverage. Moreover, Medicare being a strictly federal measure allows it to offer relatively the same services in every region of the United States (U.S. Department of Health & Human Services). Conversely, Medicaid is more of an assistance program and is constructed to serve low-income populations, regardless of patients’ ages. Both state and federal governments regulate Medicaid as a means to best assist low-income households with healthcare expenses. This includes—but is not limited to—major hospitalizations and treatments as well as routine medical care (Mitchell & Hope). Typically, patients who participate in this program have no financial obligations with regards to medical expenses—though a small co-payment may be required at times. This measure is a federal-state program, so its services vary between states (U.S. Department of Health & Human Services).
In terms of coverage, there are also differences and similarities between the two programs. For Medicare, there are several parts that each cover a specific aspect of healthcare. Medicare Part A is involved with hospital insurance and is offered without premiums to eligible patients who have paid Medicare taxes for a minimum of forty calendar quarters within their life spans (Mitchell & Potter). Part A is typically associated with skilled nursing care, hospital services, hospice services, and home healthcare. Patients ineligible for Part A oftentimes have the option of purchasing it. In contrast, Medicare Part B is associated with medical insurance and covers outpatient hospital care, physician services, and other comparable services that are traditionally covered in typical health insurance plans. In addition, the combination of Parts A and B is often referred to as Original Medicare. Medicare Part C, otherwise known as Medicare Advantage, is run by approved private insurers and includes all the benefits included in Medicare Parts A and B (Masterson). For all the above-mentioned plans, patients have the option of purchasing other benefits, including those involving dental, vision, and prescription drug coverage. Lastly, Medicare Part D involves prescription drug payments only. Individuals can automatically enroll in Medicare as soon as they turn 65, but if individuals choose to delay enrollment, possibly due to already being insured by an employer or other organization, these individuals must manually enroll later on. However, for Medicare Parts C and D, individuals must sign up once they become eligible or during specific annual enrollment periods. The State Health Insurance Assistance Program, or SHIP, serves to inform and educate people who are eligible for Medicare about their options and the diverse kinds of coverage offered. This service also aids beneficiaries in applying to other programs, including Medicaid (Mitchell & Potter).
Medicaid involves a similar distinction regarding benefits issued and covered since these benefits vary based on the issuing state. However, the following benefits are included in every program: lab and X-ray services, inpatient and outpatient hospital services, family planning services (such as birth control and nurse-midwife services), health screenings, applicable child medical treatments, nursing facility services for adults, and adult surgical dental services (Mitchell & Potter).
Additionally, certain individuals are eligible for both programs due to concurrent disability benefits. As an example, these individuals could have the Original Medicare (Parts A and B) or a Medicare Advantage plan (Part C). Medicare would subsequently cover prescription drugs under Part D, while Medicaid covers other forms of care and medications that Medicare does not. Thus, having both programs would allow individuals to cover most of their healthcare costs (Mitchell & Potter).
As such, Medicare and Medicaid are two distinct U.S. government programs that are designed to aid different populations in gaining access to the healthcare they need.
1Deductible: The amount you pay for covered health care services before your insurance plan starts to pay. With a $2,000 deductible, for example, you pay the first $2,000 of covered services yourself. After you pay your deductible, you usually pay only a copayment or coinsurance for covered services (Healthcare.gov).
2Premium: The amount you pay for your health insurance every month (Healthcare.gov).
Bibliography
Masterson, Les. “Medicare vs Medicaid – What Is the Difference between Medicare and Medicaid?” Insure.com, 15 June 2020, www.insure.com/health-insurance/key-differences-between-medicare-and-medicaid.
Mitchell, Jennifer, and Daniel Potter. “Medicare vs. Medicaid.” Healthline.com, Healthline Media, 10 Dec. 2019, www.healthline.com/health/medicare/medicare-vs-medicaid#disability.U.S. Department of Health & Human Services. “What Is the Difference between Medicare and Medicaid?” HHS.gov, 2 Oct. 2015, www.hhs.gov/answers/medicare-and-medicaid/what-is-the-difference-between-medicare-medicaid/index.html.
To Our Modern Day Superheroes
PMHS Statement – BLM